|
|
synonyms: calcific tendinitis, calcifying tendinitis, hydroxyapatite deposition disease, HADD, calcium rotator cuff
Calcific Tendinitis ICD-10
Calcific Tendinitis ICD-9
- 726.11 (calcifying tendinitis of the shoulder)
Calcific Tendinitis Etiology / Epidemiology / Natural History
- Idiopathic calcium deposition (accumulation of basic calcium phosphate crystals (hydroxyapatite) within the rotator cuff.
- Natural history: strong tendancy for spontaneous resorption with tendon reconstitution.
- Consists of formative(most painful) and resorptive phases.
- Women > men, Mean age of onset = 43.5 yers, 22.% bilateral, generally overweight with low levels of alcohol consumptions. (Harvie P, JSES 2007;16:169).
- Associated with endocrine (hypthyroidism), autoimmune and hormone-related gynecologic disorders (Harvie P, JSES 2007;16:169). Patients with associated disorders have poorer outcomes.
Calcific Tendinitis Anatomy
- Most commonly affects the supraspinatus, but can affect infraspinatus, subscapularis.
- See also Shoulder Anatomy.
Calcific Tendinitis Clinical Evaluation
- Anterosuperior shoulder pain may have radiation to deltoid origin.
- More painful in formative stage.
- Physical exam is typically similar to that of Subacromial Impingement 726.10.
Calcific Tendinitis Xray / Diagnositc Tests
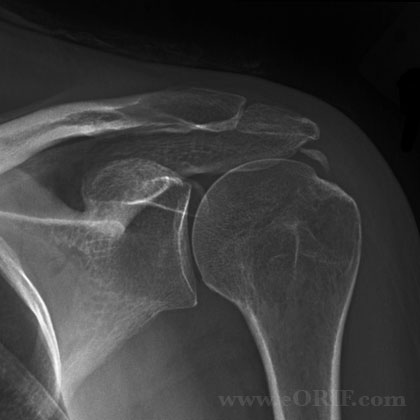
- AP, scapular lateral and axillary views. AP-IR and AP-ER often helpful and demonstrate calcification within the RTC tendons.
- Consider lab test for hypothyroidism.
- Ultrasound is sensitive in detecting calcium deposits and helpful for pre and post-op evaluation. (Teefey SA, JBJS 2000;82A:498).
Calcific Tendinitis Classification / Treatment
- 72.7% of patients treated non-operatively are satisfied with outcome, 85.4% of patients treated with operative excision are satisfied with outcome. Non-operative treatment fails in 46.9% of patients with endocrine disorders and in 22.7% of patients without endocrice disorders (Harvie P, JSES 2007;16:169).
- Classification: Type A=dense, rounded and sharply delineated calcifications. Type B=multilobular, radiodense, sharply delineated. Type C=more radilolucent and heterogeneous with irregular outlines. Type D=dystrophic calcific lesions of the tendon insertion.
- Initial treatment = conservative observation, pain can frequently be improved with sub-acromial steriod injection. NSAIDs, ROM exercises.
- Treatment options: extracorporeal shock waves 70% successful (Daecke W, JSES 2002;11:476), percutaneous needle aspiration and lavage, arthroscopic excision (Porcellini G, JSES 2004;13:503).
- Arthroscopic Excision Technique: see Shoulder Arthroscopy. After subacromial bursectomy the calcium deposits are located by percutaneous needling based on pre-operative xrays. Calcium deposits are then removed generally with a full-radius resector and curettes. Any residual RTC tears are then repaired in standard fashion, often RTC tears can be repaired by side-to-side suturing. Outcome is dependent on complete removal of calcium deposits. (Porcellini G, JSES 2004;13:503).
Calcific Tendinitis Associated Injuries / Differential Diagnosis
Calcific Tendinitis Complications
- Residual calcium deposits with continued pain.
- RTC tear
- Infections
- Stiffness
- Complex Regional Pain Syndrome 337.21
- Nerve injury: Axillary nerve, Brachial plexus
- Fluid Extravasation:
- Chondrolysis: though to be related to heat from electo cautery or radiofrequency probes used during capsular release or capsular shrinkage.
- Hematoma
- Chondral Injury / arthritis
Calcific Tendinitis Follow-up Care
- Post-op: Shoulder immobilizer, Begin elbow/wrist/hand active and passive ROM immediately. Shoulder Pendelum ROM exercises.
- 7-10 Days: Start physical therapy with PROM, consider AROM depending on any residual RTC tear that needed repairing
- 6 Weeks: Discontinue sling, progress with AROM.
- 3 Months: Progress with strengthening.
- 6 Months: Progressive strengthening, gradual return to normal activities. Home program.
- 1Yr: Assess outcomes, patient satisfaction.
- Outomes of Arthroscopic excision: Mean Constant score increased from 55.1 pre-op to 86.4 post-op. Outcomes dependent on amount of residual calcium after excision. (Porcellini G, JSES 2004;13:503).
Calcific Tendinitis Review References
|

