|
|
synonyms:essex-lopresti, radial head fracture, elbow dislocation, radioulnar joint dislocation
Essex-Lopresti ICD-10
Essex-Lopresti ICD-9
- 813.05(closed fracture of head of radius)
- 833.01 (closed dislocation, radioulnar joint, distal)
Essex-Lopresti Etiology / Epidemiology / Natural History
- Radial head fracture or dislocation with complete disruption of the interosseous membrane and TFCC.DRUJ allowing proximal migration of the radius. (Esses-Lopresti P, JBJS 1951;33B;244).
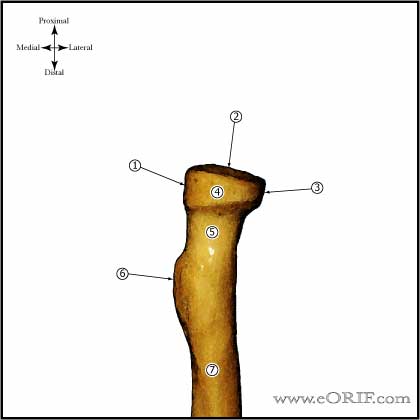
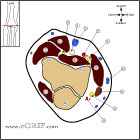
Essex-Lopresti Anatomy
- Primary stabilizer preventing proximal migration of the radius = the radial head. Secondary stabilizers = the interosseous ligament and the triangular fibrocartilage.
Essex-Lopresti Clinical Evaluation
Essex-Lopresti Xray / Diagnositc Tests
- A/P, lateral and oblique elbow views and P/A, lateral and oblique wrist views indicated.
- Radiocapitellar view is accomplished by positioning the patient as for a lateral x-ray view but angling the tube 45° toward the shoulder
- Elevation of the anterior and postior fat pads(sail sign) indicates intraarticular hemarthrosis and may indicate non-displaced fx. Anterior fat pads are commonly seen. Posterior fat pad sign is associated with intraarticular fracture.
- Bilateral PA views of both wrists in neutral rotation should be obtained to evaluate ulnar variance in patients with wrist pain.
- CT can better delineate fracture configuration, but is generally not needed. 3D reconstructions can greatly enhance the pre-operative plan for complex fractures.
Essex-Lopresti Classification / Treatment
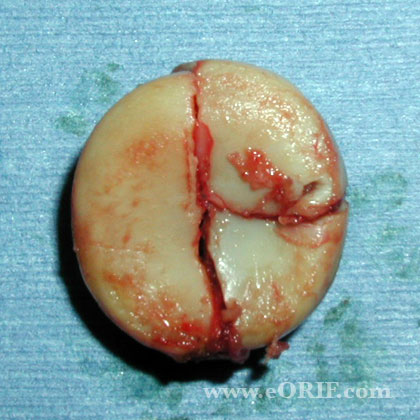
- Acute: Treatment = Radial Head Fracture ORIF if possible, with immobilization of the forearm in supination. Comminuted non-repairable radial head fractures require Radial Head Replacement. May consider cross-pinning of the ulna (in suppination), or direct TFCC Tear.
- Chronic: patients which develope proximal migration of the radius following radial head excision. No recommened treatment has been established. Consider allograft radial head replacement (Szabo RM, J Hand Surg 1997;22A:269), or metal radial head replacement. Ulnar variance must be restored at surgery for optimal outcomes.
Essex-Lopresti Associated Injuries / Differential Diagnosis
Essex-Lopresti Complications
- Contracture / stiffness(generally lack full extention)
- Wrist pain (interossious ligament / DRUJ Instability / TFCC Tear).
- Posttraumatic arthritis
- Instability
- Heterotopic Ossification
- Reported complications with radial head excision include loss of grip strength, pain at the wrist, valgus instability and posttraumatic arthritis of the trochlear-olecranon articulation.
- AVN
- Nonunion: (Ring D, CORR 2002;398:235).
- Painful Hardware
Essex-Lopresti Follow-up Care
- Post-op: Splint with forearm in supination or neutral. Start early active range of motion as soon as possible. Consider Indomethacin 75mg QD/NSAIDs for patients with complex dislocations or Radial head replacement for HO reduction.
- 7-10 Days: Evaluate incision, remove stitches, Begin early active range of motion as soon as possible. Consider hinged elbow brace for high energy injuries/instability. Start physical therapy. Avoid flexion in pronation. Patients with Essex-Loprestic injuries are held in full supination for 3-4 weeks.
- 6 Weeks: Consider static progressive nightime extension splinting if a flexion contracture is present 6 weeks after injury. 10° to 15° flexion contractures are not uncommon. If DRUJ treated by pinning remove pins at 6wks.
- 3 Months: Progress with ROM. May take 6-12 months to regain ROM. Begin sport specific therapy.
- 6 Months: May return to full activities provided patient is asymptomatic
- 1Yr: Assess outcomes, repeat xrays.
- Radial Head Rehab Protocol.
- See also Elbow Outcome Measures.
Essex-Lopresti Review References
- Trousdale RT, JBJS 1992;74A:1486
- Rockwood and Green's Fractures in Adults 6th ed, 2006
- Advanced Reconstruction-Elbow, AAOS 2007
|



