|



|
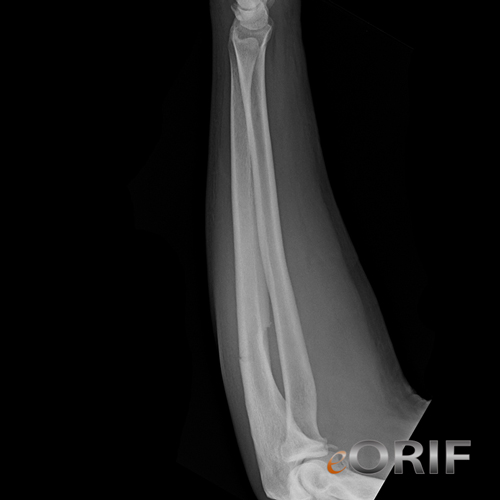
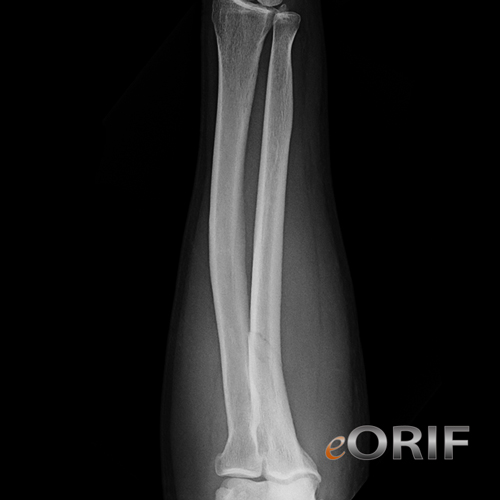
synonyms: nightstick fracture, forearm fx, ulnar shaft fracture, ulna fracture
Ulnar Shaft Fracture ICD-10
- S52.91XA : Unspecified fracture of right forearm , initial encounter for closed fracture
- S52.92XA : Unspecified fracture of left forearm , initial encounter for closed fracture
- S52.209A : Unspecified fracture of shaft of unspecified ulna, initial encounter for closed fracture
- S52.209B : Unspecified fracture of shaft of unspecified ulna, initial encounter for open fracture type I or II
- S52.209C : Unspecified fracture of shaft of unspecified ulna, initial encounter for open fracture type iliA, IIIB, or IIIC
- S52.279A : Monteggia's fracture of unspecified ulna, initial encounter for closed fracture
- S62.90XA : Unspecified fracture of unspecified wrist and hand, initial encounter for closed fracture
- S62.90XB : Unspecified fracture of unspecified wrist and hand, initial encounter for open fracture
Ulnar Shaft Fracture ICD-9
- 813.22(closed, ulna fracture alone)
- 813.32(open, ulna fracture alone)
Ulnar Shaft Fracture Etiology / Epidemiology / Natural History
- Most fractures of the ulnar shaft are caused by direct blows and result in minimal soft-tissue injury.
Ulnar Shaft Fracture Anatomy
Ulnar Shaft Fracture Clinical Evaluation
Ulnar Shaft Fracture Xray / Diagnositc Tests
- A/P and Lateral of radius/ulna to include elbow and wrist
- Separate views of wrist and elbow if indicated
- Template before case
Ulnar Shaft Fracture Classification / Treatment
- "Non-Displaced" Middle 1/3 (<50%displacement, <10° angulation): functional fracture brace or long arm cast. Ensure distal radioulnar joint is reduced.
- Displaced Middle 1/3 (>50%displacement, >10° angulation): ORIF
- Proximal 1/3: ORIF, even non-displaced fractures have high propensity to displace with time.
- Non-Displaced Distal 1/3 (<5%displacement, <2° angulation): displacement in the distal 1/3 is poorly tolerated. Functional fracture brace or long arm cast if truely nondisplaced. Ensure distal radioulnar joint is reduced.
- Displaced distal 1/3: ORIF
- ORIF: 8 cortices above and below recommended
- Nonsurgical treatment leads to a high rate of union and a good functional outcome. (Zych GA, CORR 1987;219:194).
- AO Classification
- Open Fracture Classification
Ulnar Shaft Fracture Associated Injuries / Differential Diagnosis
Ulnar Shaft Fracture Complications
- Superficial wound infection
- contracture
- Nonunion: (incidence is higher for comminuted or displaced fx's)
- Hardware failure
- Malunion
- Painful Hardware
- Ulnar nerve palsy
- Radial nerve palsy
Ulnar Shaft Fracture Follow-up Care
- Post-op: Volar plaster splint with sling. NWB. Active elbow and finger ROM.
- 7-10 Days: Wound check, Place in funtional brace (interosseous mold). Begin active pronation/supination. Continue active elbow and finger ROM. Activity restrictions. Use for arm for light ADLS only. NWB.
- 6 Weeks: Gradually resume normal activites provided bony union is evident on xrays.
- 3 Months: Consider bone stimulator if union is not evident on xray.
- 6 Months: return to sports / full activities.
- 1Yr: Follow-up xrays, assess outcomes.
Ulnar Shaft Fracture Review References
|





