|
|
synonyms: Tennis Elbow, lateral epicondylitis, common extensor tear, common extensor tenosynovitis, extensor carpi radialis brevis tear
Lateral Epicondylitis ICD-10
Lateral Epicondylitis ICD-9
- 726.32 (lateral epicondylitis)
Lateral Epicondylitis Etiology / Epidemiology / Natural History
- Pain at the lateral epicondyle which often radiates into the forearm and is typically insidious in onset. Usually hx of repetitive activity.
- Associated with tennis, squash, fencing, meat cutting, plumbing, painting, raking, weaving
- Believed to be initiated by a microtear, most often within the origin of the extensor carpi radialis brevis. May originate in any muscle originating from the epicondyle
- Angiofibroblastic hyperplasia of involved tissue demonstrating fibroblast proliferation, neovascularization and hyaline degeneration without acute inflammatory cells. (Regan W, AJSM 1992;20:746)
- Male = female
- Incidence is 2-3.5 times greater in tennis players with over 2hrs of racket time per week than those with less than 2 hrs per wk (Gruchow HW, AJSM 1979;7:234).
- Affects 10-50% of tennis players (Jobe FW, JAAOS 1994;2:1).
- Typically 4th to 5thdecade
- Affects 1-3% of adults/year.
- More common in dominant arm.
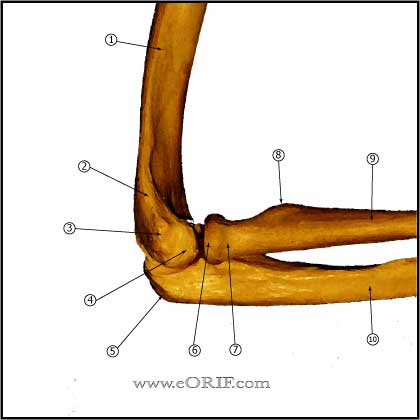
Lateral Epicondylitis Anatomy
Lateral Epicondylitis Clinical Evaluation
- Tenderness over the extensor tendon origin, usually localized to the ECRB portion.
- Maximal tenderness usually 2-5mm distal and anterior to the midpoint of the lateral epicondyle
- Resisted wrist and finger extension with the elbow in full extension exacerbates pain
- Normal wrist/elbow ROM
- If pt has pain on resisted suppination consider PIN irritation as cause.
Lateral Epicondylitis Xray / Diagnositc Tests
Lateral Epicondylitis Classification / Treatment
- Initial Treatment
-Cessation of offending activity is required initially.
-Avoid immobilization/inactivity which leads to disuse atrophy
-Ice 20minutes 3-4x/day
-NSAIDs for 10-14 days
-Counterforce brace placed over the forearm musculature; questionable benefit (Struijs PA, AJSM 2004;32:462).
-Dynamic extensor bracing has shown statistically significant benefits (Faes M, CORR 2006;442:149).
- Secondary Treatment
-corticosteriod injection deep to ECRB, anterior and distal to the lateral epicondyle into fatty subaponeurotic recess. SQ injection-SQ atrophy
-Corticosteriod injection=55-89% pain relief: 18-54% recurrence. (Beller E, BMJ 2006;333:939). Provides short term benefit, but may be detrimental in the long term (Bisset L, BMJ 2006;333:939).
-Platelet-Rich Plasma injection. 81% improvement in VAS score at 6 months (Mishra A, AJSM 2006;34:1774).
-Ultrasound, high-voltage galvanic stimulation no prospective randomized trials
-Botulinum Toxin A: shown to have short-term benefit (Placzek R, JBJS 2007;89A:255).
- Final Treatment
-If fails 6-12 months of non-operative treatment consider Lateral Epicondyle Debridement., Percutaneous technique (Dunkow PD, JBJS 2004;86Br:701), arthrocsopic debridement.
- Botulinum toxin injection has not been shown to be of benefit (Hayton MJ, JBJS A 2005;87:503-507).
- Shock wave therapy / ESWT has little or no benefit (Buchbinder R, Cochrane Database Syst Rev 2005;4:CD003524).
Lateral Epicondylitis Associated Injuries / Differential Diagnosis
Lateral Epicondylitis Complications
- Persistent pain of varying degree
- Infection
- Residual strength deficit
- Functional limitations
- Joint instability
Lateral Epicondylitis Follow-up Care
- Lateral Epicondylitis Rehab Protocol: wrist extensor stretching and progressive isometric exercises. Later begin eccentric and concentric exercises
- 26% of patients will have recurrence of symptoms and over 40% have prolonged minor discomfort. Other more optomisitic reports show 85-90% successful nonoperative treatment
- Surgery=posterior mold for 7-10days. Then progressive mobilization/gentle passive and active elbow, wrist, hand motion. Counterforce bracing for 3-6 months. Resisted isometrics at 4wks, progressive strengthening at 6 wks. Return to lifting/athletics usually by 3-4 month.
Lateral Epicondylitis Review References
|


