 |
synonyms:revision THA, total hip arthroplasty revision, total hip replacement revision
Revision THA CPT
Revision THA Indications
- Aseptic loosening
- Recurrent dislocation
- Sepsis (periprosthetic infection)
Revision THA Clinical Evaluation
- Pain (initially at night/rest), fever, chills, draining sinus tracts. Symptoms may be mild and difficult to differentiate between asceptic loosening, instability, etc.
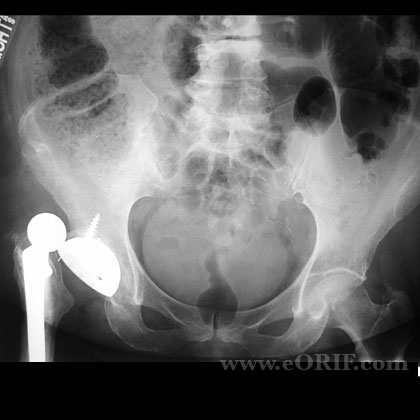
Revision THA Xray / Diagnositc Tests
- Xrays: evaluate for periosteal reaction, scattered foci of osteolysis, bone resoprtion, implant wear, progressive radiolucencies, osteopenia, .
- Pedestal sign: endosteal new bone formation below the distal end of the stem. Implies prosthesis-to-bone stress transfer away from the porous coating metaphyseal part of the stem and is associated with instability especially if there is lucency around the stem proximally.
- Bone Scan: sensitivity = 33%, specificity = 86%, positive predictive value = 30%, negative predictive value = 88% for infection. (Levitsky KA, J Arthroplasty. 1991;6:237)
- ESR (Westergen erthrocyte sedimentation rate): rises normally after total joint surgery. Returns to normal 6 weeks after surgery. Infection suggested if elevated 3 months after surgery.
- CRP (C-reactive protein): Rises normally after total joint surgery. Returns to normal @3weeks after surgery. Infection suggested if elevated 3 months after surgery.
- Interleukin-6 (IL-6): Rises normally after total joint surgery. Returns to normal within 48 hours after surgery. Elevated (>10 pg/mL [>10 ng/L]) in patients with periprosthetic infection.
- Aspiration of Joint fluid: send for aerobic culture anaerobic culture, sensitivities, Gram stain, acid-fast staining, CBC with differential. Leukocyte count > 1.7x109/L indicates infection.
Metal-on-metal Total Hip Arthroplasty (MOM)
- Metal-on-metal articulation: excellent wear rates in vitro.
- Local soft-tissue reactions, pseudotumors, and potential systemic reactions: renal failure, cardiomyopathy, carcinogenesis
- Histology of metal-on-metal (MOM) hip arthroplasties / pseudotumor: predominantly tissue necrosis with infiltration of lymphocytes and plasma cells.
- Relatively contraindicated in women of child-bearing age; potential teratogenesis (metal ions may transfer across the placental barrier)
- Painful metal-on-metal THA: ESR, CRP, and serum cobalt and chromium ion levels, MARS MRI(fluid collections, pseudotumors, and abductor mechanism destruction). Hip arthrocentesis indicated if CRP is elevated to eval for concomitant infection. Manual cell count and differential required do to potential falsely elevated cell counts with automated systems.
- Elevated serum metal ions and abductor dysfunction, suggests poor bearing function and adverse local tissue reaction (ALTR).
- Cobalt disproportionately higher than chromium suggests corrosive changes at the prosthetic femoral neck (trunnionosis).
- Instability is the most common complication following revision of failed metal-on-metal hip replacements.
- Generally do not remove a stable cementless femoral stem. If revising for metalosis or there is some damage to the taper use a titanium taper sleeve with a ceramic ball. Use of a ceramic head on a previously used trunnion risks fracture of the ceramic head.
Ceramic-on-Ceramic THA revision
- Ceramic-on-ceramic THA should be revised to ceramic-on-ceramic components due to remaining ceramic particles from the primary implant which can lead to severe abrasion in non-ceramic-bearing surfaces. (Rambani R, Kepecs DM, Mäkinen TJ, Safir OA, Gross AE, Kuzyk PR. Revision Total Hip Arthroplasty for Fractured Ceramic Bearings: A Review of Best Practices for Revision Cases. J Arthroplasty. 2017 Jun;32(6):1959-1964. doi: 10.1016/j.arth.2016.12.050.)
Revision THA Classification / Treatment
- Femoral Bone Loss - Paprosky Classification
-Type 1: minimla metaphyseal involvement and adequate cancellous bone. RX: 6in long primary fully porous-coated stem.
-Type 2: metaphyseal damage with a minimally involved diaphysis. RX: 6in long primary fully porous-coated stem.
-Type 3A: metadiaphyseal damage with 4cm of reliable cortex proximal to the isthmus. RX: 7-10in long revision fully porous-coated stem.
-Type 3B: metadiaphyseal damage with 4cm of reliable cortex distal to the isthmus. RX: 7-10in long revision fully porous-coated stem.
-Type 4: extensive metadiaphyseal and thin ballooned cortices with widened canals precluding reliable fixation. RX: impaction grafting, modular tapered stems, allorgraft prosthetic composites, megaprosthesis.
- Impaction bone grafting (Schreurs BW, JBJS 2006;88A:259)
- Localized osteolytic lesion with well-fixed acetabular shell (possible eccentric acetabular wear): removal of acetabular screw with debridement of osteolytic lesion and bone grafting with exchange of acetabular shell. (Mall NA, CORR 2010:468:3286-3294).
- Acetabular Bone Loss - Paprosky Classification
-Type 1: rim and columns intact with more than 50% of the cup in contact with host bone. RX: allograft filling of contained defects with press-fit cup supplemented with screws.
-Type 2A: anterior and posterior columns intact, partial loss of the superomedial wall. RX: allograft filling of contained defects with press-fit cup supplemented with screws.
-Type 2A: anterior and posterior columns intact, partial loss of the superolateral wall. RX: allograft filling of contained defects with press-fit cup supplemented with screws.
-Type 2A: anterior and posterior columns intact, partial loss of the medial wall. RX: allograft filling of contained defects with press-fit cup supplemented with screws.
-Type 3A: severe bone loss involving the acetabular walls and pelvic columns. Rx: bulk allograft with antiprotrusio cages or porous tantalum metal augmentations. (Sporer SM, J Arthroplasty 2006;21S:83).
-Type 3B: severe bone loss involving the acetabular walls and pelvic columns with pelvic discontinuity. Rx: bulk allograft with antiprotrusio cages or porous tantalum metal augmentations. (Sporer SM, J Arthroplasty 2006;21S:87).
- Posterior column fractured or disrupted: fixation with a reconstruction plate and/or the use of an antiprotrusio cage is recommended.
- Hip Antibiotic Spacers: Biomet Stage One; Exatech hip antibiotic spacer.
- Extended trochanteric osteotomy (transfemoral approach) is generally recommended for revision of femoral stems due to risks of proximal femoral fracture with stem removal without osteotomy. Osteotomy facilitates atraumatic removal of the stem and cement. (Jando VT, Instr Course Lect. 2005;54:143-55). Extended trochanteric osteotomy reduces torsional strength by 73% even when the osteotomy fragment is repaired. Bone mineral density directly affects absolute femoral strength. (Noble AR, J Bone Joint Surg Am 2005;87(3):521-529).
Revision THA Associated Injuries / Differential Diagnosis
- Periprosthetic infection
- Mechanical failure
- Dislocation
- Death (cardiac / pulmonary)
- Nerve palsy (peroneal, sciatic, femoral)
- Vascular injury (femoral, iliac, obturator
- DVT/PE
- Leg-length discrepancy
Revision THA Complications
Revision THA Follow-up Care
Revision THA Review References
- Sporer SM, CORR 2003;417:203
- Kwon YM, Jacobs JJ, MacDonald SJ, Potter HG, Fehring TK, Lombardi AV. Evidence-based understanding of management perils for metal-on-metal hip arthroplasty patients. J Arthroplasty. 2012 Sep;27(8 Suppl):20-5.
- Peterson CA, Lewallen DG: Periprosthetic fracture of the acetabulum after total hip arthroplasty. J Bone Joint Surg Am 1996;78:1206-1213.
- Berry DJ: Antiprotrusio cages for acetabular revision. Clin Orthop Relat Res 2004;420:106-112.
|

