|



|
synonyms: tibial shaft malunion,
Tibial Malunion ICD-10
Tibial Malunion ICD-9
- 733.81 (Malunion of fracture)
- 733.82 (Nonunion of fracture, pseudoarthrosis)
Tibial Malunion Etiology / Epidemiology / Natural History
- >5° angulation has been shown to cause subjective complaints and functional limitations (Kyro A, Ann Chir Gynaecol 1991;80:294).
- Tibial malunion leads to degenerative changes in the knee and ankle (van der Schoot DK, JBJS 1996;78Br:722).
- Coronal plan angulation alters lower extremity alignment anc can contribute to ligamentous laxity.
Tibial Malunion Anatomy
- Size ranges from 30-47cm in adults, intramedullary diameter =8-15mm
- Proximal tibia has average 15 degree apex anterior angulation
- Radius of supramalleolar curvature is approximately 20cm, ie medial surface turns medially @25degrees.
- Diaphyseal blood supply is via a single nutrient artery, the proximal branch of the posterior tibial artery which passes through the most proximal portion of the tibialis posterior to obliquely enter the tibial shaft on its posterior surface in the proximal portion of the middle third of the bone. Only peripheral 1/3-1/4 of diaphyseal cortex is supplied by periosteal vessels.
- Fibula bears 6-17% of body weight, fibular head is attachment for LCL and biceps femoris, common peroneal nerve wraps around fibular neck.
- Interosseous membrane fibers run downward and laterally
Tibial Malunion Clinical Evaluation
- Evaluate limb alignment and knee /ankle ligamentous exam
- Document NVexam
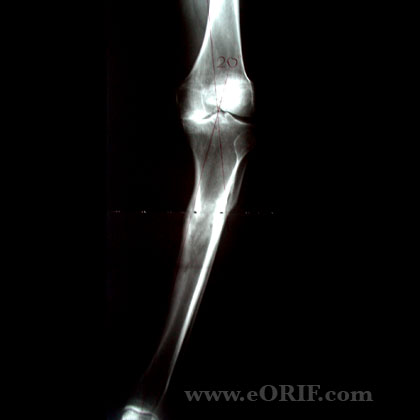
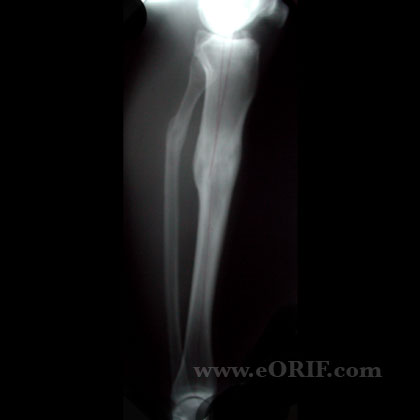
Tibial Malunion Xray / Diagnositc Tests
- Full-length standing xrays with beam centered at the knee (beam directed at the patella from @10ft away) indicated to determine mechanical axis and joint orientation.
- A/P and lateral views of the tibia.
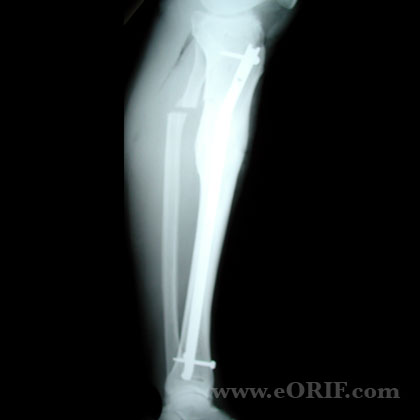
Tibial Malunion Classification / Treatment
- Nonsurgical: unloading knee braces, shoe orthoses, shoe lifts, NSAIDs.
- Surgical correction is indicated for: ligamentous instability on the convex side of the deformity, leg-length discrepancy >2cm, inability to place the foot in a plantigrade position, unicondylar knee arthritis, >10° varus deformity at knee or ankle, >15° valgus deformity at knee or ankle, or 20mm medial shift in the mechanical axis.
- Closing wedge osteotomy
- Opening wedge osteotomy
- Dome osteotomy
- Oblique cut osteotomy: (Rab GT, JPO 1988;8:715), (Sanders R, JBJS 1995;77A:240), (Sangeorzan BJ, JOT 1989;3:267), (Sanders R, JBJS 1996;78:151).
- Distraction Ostogenesis: (Tetsworth KD, CORR 1994;301:102).
- Talor Spatial frame (Feldman DS, JOT 2003;17:549).
- Clamshell Osteotomy: (Russell GV, JBJS 2009;91A:314).
Tibial Malunion Associated Injuries / Differential Diagnosis
- Knee arthritis
- Ankle arthritis
Tibial Malunion Complications
- Nonuion
- Malunion
- Wound dehiscence
- Hardware failure
- Peroneal Nerve palsy
- Compartment Syndrome
Tibial Malunion Follow-up Care
- Post-op: Apply bulky Jones dressing with posterior mold to avoid equinus contracture. Elevate. Consider DVT prophyaxis.
- 7-10 Days: Remove splint, wound check. WBAT, PT, knee, ankle mobilization based on fracture stability / soft tissues.
- 6 Weeks: Xrays. Advance PT
- 3 Months: Xrays. Consider bone stimulator/nail dynamization if union is not evident. Sport specific PT.
- 6 Months: Return to full activities
- 1Yr: follow-up xrays, asssess outcomes.
Tibial Malunion Review References
- Probe RA, JAAOS 2003;11:302
- °
|






