|
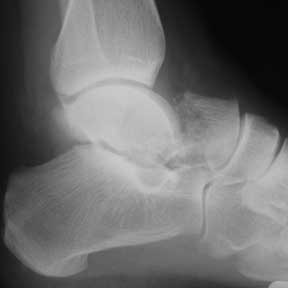
synonyms: Astragalus fracture, talus fracture, talar neck fracture Talus Fracture ICD-10
Talar Neck Fracture Etiology / Epidemiology / Natural History
Talar Neck Fracture Clinical Evaluation
Talar Neck Fracture Classification / Treatment
Talar Neck Fracture Associated Injuries / Differential Diagnosis
Talar Neck Fracture Complications
Talar Neck Fracture Follow-Up care
|