|
|
synonyms:
ORIF Pelvic Ring CPT
ORIF Pelvic Ring Indications
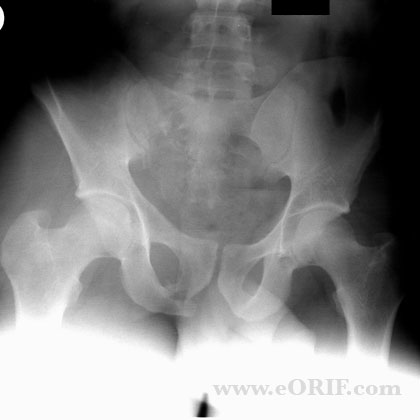
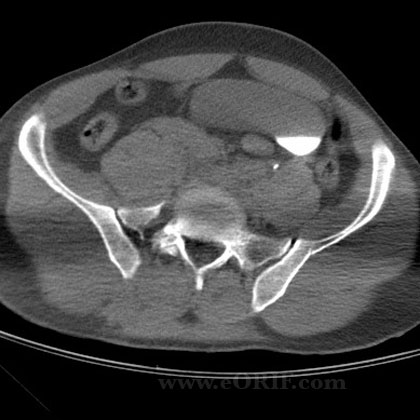
- Unstable pelvic ring injuries (SI joint dislocations, sacral fractures, etc)
ORIF Pelvic Ring Contraindications
- Dysmorphism of the upper sacrum precludes iliosacral screws.
- Obesity (iliosacral screw placement)
- Soft tissue injury
- Patients with abdominal / urologic contrast agents on board.
ORIF Pelvic Ring Alternatives
- Nonoperative management, skeletal traction
ORIF Pelvic Ring Planning / Case Card
- High-quality fluoro images of the entire pelvis must be varified before starting the surgery.
- Distal femoral traction improves reduction.
- At least 1cm must be available between the foramina on three sequential preop CT slices (cmm slices( for safe S2 sacral screw placement. (Moed BR, JOT 2006;20:378).
ORIF Pelvic Ring Technique
- prone OSI table
- vertical incision 1-2cm lateral to PSIS, from iliac crest to greater sciatic notch
- reflect gluteus maximus to reveal greater sciatic notch, PIIS,inferior sacroiliac joint, piriformis(origin=lateral mass of sacrum)
- sacrotuberous ligament, erector spinae, multifidus muscle,
- allows visualization of ilium, sacroiliac joint, posterior sacrum
- stronqest fixation seems to be iliosacral screws. 6.5-7mm cancellous screw into S1 body. Starting point on ilium is alonq a line running from iliac crest to greater sciatic notch @15mm anterior to and paralleling the crista glutea. 2 screws preferred. Optimal distance from crista glutea is 15-20mm. Risks=sacral nerve root, vessels, dura
- sacroiliac joint dislocations must undergo reduction and fixation because they are a ligamentous injury and very unlikely to heal without fixation
- Pelvic orthotic devices / binders can remain in place for up to 190 hours without causing soft tissue compromise (Krieg JC, J Trauma 2005;59(3):659-664).
ORIF Pelvic Ring Complications
- Infection
- Poor wound healing
- Chronic Osteomyelitis
- Pain
- Painful hardware
- Loss of reduction
- Nonuion
- Limb length discrepancy
- Sitting imbalance
- Gait disturbance
- DVT / PE
ORIF Pelvic Ring Follow-up care
- Post-op: 24hrs antibiotic, SCDs, Ted hose, Partial weight bearing. Review reduction on post op A/P pelvis, inlet and outletviews.
- 7-10 Days: Wound check. Continue partial/non weight bearing
- 6 Weeks: Advance weight bearing gradually. Review A/P pelvis, inlet and outletviews.
- 3 Months: Review A/P pelvis, inlet and outletviews.
- 6 Months: Return to labor. Review reduction on post op A/P pelvis, inlet and outletviews. Obtain follow-up CT scan.
- 1Yr:Assess outcome. Review A/P pelvis, inlet and outlet views.
ORIF Pelvic Ring Outcomes
- NO intraoperative nerve damage, 4% loss of reduction for S2 iliosacral screws(Moed BR, JOT 2006;20:378).
- Good outcome studies are lacking. Outcomes are dependent on initial displacement, neurologic injury, urologic injury and adequacy of reduction.
ORIF Pelvic Ring Review References
- Starr AJ, Chapter 41, Rockwood and Greens.
- Olson SA, ICL 2005;54:383
- °
|