|
|
Synonyms: OCD, osteochondritis dissecans, osteochondral defect, osteochondral lesion
OCD ICD-10
OCD ICD-9
- 732.7(osteochondritis dissecans)
OCD Etiology / Epidemiology / Natural History
- OCD = a localized injury or condition affecting an articular surface that involves separation of a segment of cartilage and subchondral bone. (Schenck RC Jr, LBLS 1996; 78A: 439)
- Generally age 10-15, although can occur at any age.
- Male/female = 5/3
- 15-30% bilateral (Hefti F, JPO B 1999; 8: 231)
- Etiology unknown: repetitive microtrauma vs vascular insufficiency vs inherited factors.
- Skeletal age at onset is most important factor in determining prognosis. Adult OCD lesions have very limited capacity to heal and are typically progessive. Juvenile OCD lesions with an intact articular surface have a potential for healing with cessation of repetitive impact loading activities.
OCD Anatomy
- 51% involve the lateral aspect of the medial femoral condyle; 19% central MFC; 7% medial aspect of MFC; 17% lateral femoral condyle; 7%patella; and 0.2% tibial plateau.(Hefti F, JPO B 1999; 8: 231)
OCD Clinical Evaluation
- Vague intermittent knee pain, often anterior; generally related to activity.
- Intermittent swelling / effusion.
- May have catching, locking, giving way if loose fragment is present.
- Wilson’s test: pain reproduced with internally rotating the tibia during extension of the knee between 90° and 30°; pain releaved with tibial external rotation. In internal rotation and extension, the tibial eminence impinges on the OCD lesion, causing pain. External rotation moves the eminence away from the lesion, relieving the pain. Poor predictive value. (Conrad JM, AJSM 2003; 31: 777)
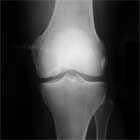
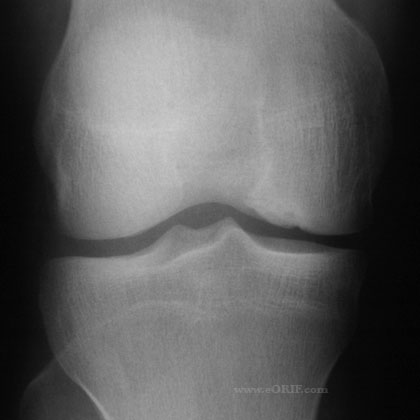
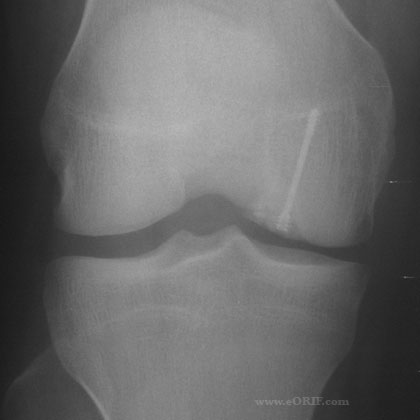
OCD Xray
- A/P, notch, and lateral views of both knees. Bilateral films indicated because of high incidence of bilateral disease. Some lesions are only visible on notch views (knee flexed 30-50 degrees). Typically appear as well circumsribed area of sclerotic subchondral bone separated fromthe remainder of the epiphysis by a radiolucent line.
- MRI: fragment instability indicated by: an area of increased homogenous signal 5 mm in diameter beneath the lesion; a focal defect 5 mm in the articular surface; and a high signal line traversing the subchondral plate into the lesion. (De Smet AA, Skeletal Radiol 1997; 26: 463)
- Bone scan may be helpful in determining prognosis. (Paletta GA Jr,ALSM 1998; 26: 7) Indicated for juvenile patients with stable lesions on xray and MRI. If the lesion is positive on bone scan, non-operative treatment is indicated.
OCD Classification / Treatment
- Lesions are generally classified radiographically by location, size, stability and skeletal age of patient.
- Location: lateral aspect of MFC, central MFC, medial aspect of MFC, lateral femoral condyle, patella
- Size: <2cm vs >2cm. Lesions >2cm have worse prognosis. (Hefti F, JPO B 1999; 8: 231)
- Stability: stable vs unstable (based on xray, MRI and physical exam findings). Fluid line between the OCD and the underlying normal bone indicates unstable.
- Skeletal age: Juvenile, Adult (based on distal femoral epiphyseal closure)
- Cahill and Berg Classification (Cahill BR, AJSM 1983; 11: 329): rarely used in clinical practive
- Juvenile Stable: non-operative treatment (activity modifications, +/- protected weight bearing, ROM exercises, acetaminophen for 3-6 months); Consider bone scan, if lesions has no uptake earlier arthroscopic intervention is indicated. Frequent follow-up with serial radiographs is important. Serial magnetic resonance images may also be useful. Consider arthroscopy if symptoms persist for six to twelve months,
- Juvenile Unstable: Arthroscopy (Kocher MS, AJSM 2001; 29: 562)
- Adult Stable: non-operative treatment for 3-6 months. Consider osteotomy if malalignment is present. Stable lesions with intact articular cartilage can be treated with subchondral drilling to stimulate vascular ingrowth (radiographic healing averags 4.4 months)
- Adult Unstable: Arthroscopy; fixation is indicated for unstable or hinged lesions. Large unstable osteochondral lesions are treated with fresh osteochondral allograft (OCA) transplantation.
OCD Arthroscopic Evaluation / Treatment
- Perform standard Knee Arthroscopy and evaluate lesion for stability and cartilage damage.
- Cartilage Intact, Stable lesion: Transchondral drilling indicated. (Kocher MS, AJSM 2001; 29: 562)
- Cartilage intact, unstable lesion: Transchondral drilling with curettage and compressive fragment fixation (Johnson LL, Arthroscopy 1990; 6: 179).Hardware removal generally done 6-12 weeks later.
- Cartilage injury, stable lesion: uncommon, consider transchondral drilling with standard chondral injury treatments.
- Cartilage injury, unstable lesion: Multiple treatment options including autologous chondrocyte implantation (Peterson L, JBJS 2003; 85Am (suppl 1): 17), mosaicplasty/OATS (Berlet GC, Arthroscopy 1999; 15: 312), and allograft OATS. Any large fragments should be fixed with or without bone graft from the proximal tibia.
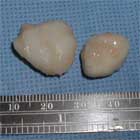
- Fragment excision is associated with poor outcomes. (Wright RW CORR 2004; 424: 239)
- Guhl’s arthroscopic staging system: Type I=softening of cartilage but no breach; type II=breached cartilage that is stable; type III=definable fragment that remains partially attached (flap lesion); type IV=loose body and osteochondral defect at the donor site. (Guhl JF, CORR1982; 167: 65)
OCD Associated Injuries / Differential Diagnosis
OCD Complications
- arthritis
- implant failure / loss of fixation
- adjacent cartilage damage from prominent hardware
- sterile abscess (biodegradable implants)
OCD Follow-up
- Post-operative patients are non–weight-bearing with range-of-motion exercises for 6 weeks.
- Hardware is generally removed arthroscopically after 6-12 weeks.
OCD Review References
- Crawford DC, Safran MR, JAAOS 2006 14: 90-100.
- Schenck RC Jr, JBJS 1996;78A:439
- Kochler MS, AJSM 2006;34:1181
- Magnussen RA, Carey JL, Spindler KP. Does operative fixation of an osteochondritis dissecans loose body result in healing and long-term maintenance of knee function? Am J Sports Med. 2009 Apr;37(4):754-9.
- DeLee & Drez's, Orthopaedic Sports Medicine: 3e; 2009

- Noyes' Knee Disorders: Surgery, Rehabilitation, Clinical Outcomes; 2009
- Insall & Scott Surgery of the Knee: Expert Consult - Online and Print, 5e, 2011

- Sherman SL, Garrity J, Bauer K, Cook J, Stannard J, Bugbee W. Fresh osteochondral allograft transplantation for the knee: current concepts. J Am Acad Orthop Surg. 2014 Feb;22(2):121-33.
- Browne JE, Branch TP. Surgical alternatives for treatment of articular cartilage lesions. J Am Acad Orthop Surg. 2000 May-Jun;8(3):180-9.
|




