|
synonyms: Jones fracture, true Jones fracture, 5th metatarsal tuberosity fracture, Jones fracture nonunion. 5th metatarsal diaphyseal stress fracture Jones Fracture ICD-10
A- initial encounter for closed fracture B- initial encounter for open fracture D- subsequent encounter for fracture with routine healing G- subsequent encounter for fracture with delayed healing K- subsequent encounter for fracture with nonunion P- subsequent encounter for fracture with malunion S- sequela
Jones Fracture Etiology / Epidemiology / Natural History
Jones Fracture Clinical Evaluation
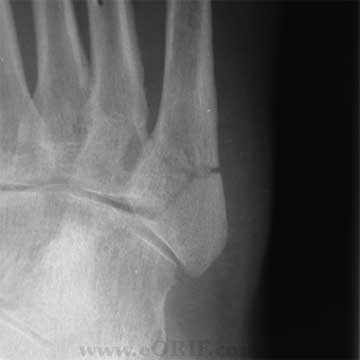
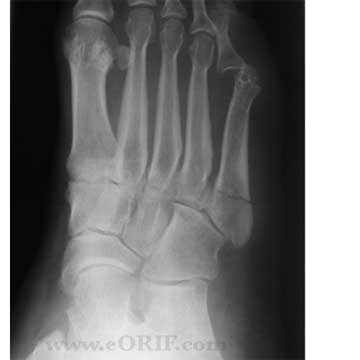
Jones Fracture Xray / Diagnositc Tests
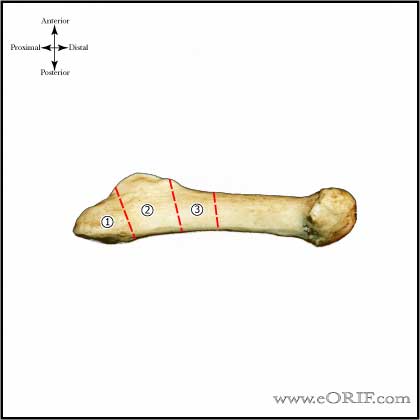
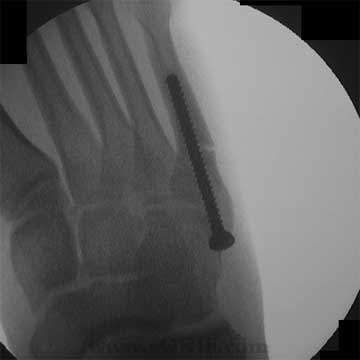
Jones Fracture Classification / Treatment
Jones Fracture Associated Injuries / Differential Diagnosis
Jones Fracture Review References
|