 |
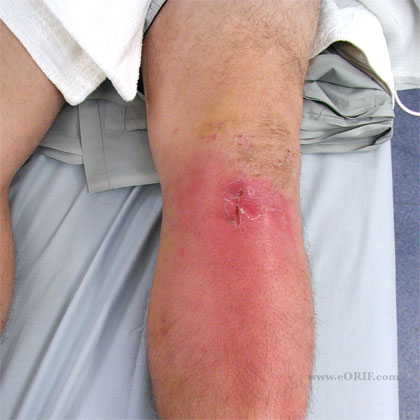
Cellulitis
- ICD-9 681.10 cellulitis, abcess unspecified
- L03.119 Cellulitis of unspecified part of limb
- spreading, diffuse inflammation, erythema, swelling and pain without abscess formation.
- Most commonly pathogens: Group A b-hemolytic Streptococcus. Also consider S aureus, MRSA. Group A strep, S Aureus, Enterobacter in diabetics.
- MRSA is becoming increaseingly prevalent, especially in hand infections. Consider Bactrim DS +/- rifampin. If group A streptococcus is strongly suspected add Keflex.
- Initial treatment: Dicloxacillin, 250-500 mg PO q6h
- Treatment non diabetics: Patients who fail to respond in 24-48 hours should be admitted and treated with IV antibiotics. Any fluctuant or questionable areas should be treated with irrigation and debridement. Nafcillin 1-2 g IV q4-6h or Cephalexin 1 g IV q8h PCN allergy: Erythromycin 250-500 mg PO q6h
- Treatment diabetics: Bactrim DX 2 tabs PO BID and Rifampin 300 mg PO BID. Severe cases: imipenem 500mg IV Q6hrs or Etrapeneum 1 g IV q24hr and vancomycin 1g IV q12hrs
Abcess
- spreading, diffuse inflammation, erythema, swelling and pain with an area of fluctuance.
- Most commonly pathogens: S aureus.
- MRSA is becoming increaseingly prevalent, especially in hand infections. Consider Bactrim DS +/- rifampin. If group A streptococcus is strongly suspected add Keflex
- Treatment: Incision and debridement. Get aerobic and anaerobic cultures and gram stain before starting antibiotics. IV antibiotics are started after cultures are taken and are adjusted based on culture results. Cefazolin 1 g IV q8h, or Ampicillin-sulbactam 1.5 mg IV q6h. Consider Nafcillin 1-2 g IV q4-6h plus gentamicin or Imipenem, 0.5-1.0 g IV q6h for IV drug abusers or diabetics with more severe abcesses.
Antibiotic cement / Antibiotic cement
- Commercially available pre-mixed antibiotic cement is low-dose and indicated for prophylaxis, not treatment of infection.
- High dose:. 3.6g tobramycin and 1g vancomycin per 40g of bone cement. (Penner MJ, J Arthroplasty 1996;11:939).
- Addition of more than 4.5 g of powder substantially weakens bone cement;
- Approx 8 grams of antibiotic powder per 40 gm of cement is the highest amount that can be added
- See also Wheeles antibiotic cement notes.
Antibiotic Beads
- 11981 Insertion, non-biodegradable drug delivery implant
- 11982 Removal, non biodegradable drug delivery implant
- 11983 Removal with reinsertion, non-biodegradable drug delivery implant
Methicillin-Resistant Staph Aureous (MRSA)
- may be hospital acquired (HA) or community associated (CA).
- infections include skin, osteomyelitis, septic arthritis, endocarditis, meningitis, pneumonia
- can be spread by direct contact, towels, sheets, wound dressings, clothes, workout areas, sports equipment, whirlpools
- Associated with contact sports: football, wrestling, rugby.
- Risk factors: artificial turf skin abrasion, shaving of skin, sharing towels or equipement, high body mass index, improperly cleaned team whirlpools.
- diagnosed by wound culture with antibiotic susceptibilities
- Treatment = Incision and drainage and antibiotics
- Empiric Treatment: Bactrim DS 1tab PO BID (8-12mg TMP/40-60SMX per kg/day divided BID for Peds); Doxyxycline 100mg PO BID(do not use in peds); Clindamycin 300-450mg PO QID (10-20mg/kg/day divided QID for PEDS); consider adding rifampin.
- Definitive antiobiotic treatment should be based on culture susceptibilities, consider Infectious disease consultation when available.
- HA-MRSA first line antibiotics: Vancomycin, consider gentamicin or rifampin for synergy. Other agents = daptomycin, linexolid, tigecycline, bactrim.
- CA-MRSA first line antibiotics: doxycycline or clindamycin, or bactrim.
- Prevention: no equipement sharing between players, no sharing towels, routine cleaning of all whirlpools / shared resources, athletes should pre-scrub with chlorhexidine soaps prior to whirlpool use, all open wounds should be occlusively dressed during practice and games,
MRSA Decolinization
- MRSA carriers (anterior nares) are 2-9 times more likely to develop surgical site infections than noncarriers
- Consider pre-op for: immunocompromised, recent nursing home/hospital admission, antibiotic exposure within 1 yr.
- Options: Chorhexicine 2% topical wash QD for 3-7 days: Doxycycline 100mg PO BID x 7 days: Mupirocin 1cm applied to nares TID for 5-7 days: Providone-Iodine 5% 4x per day for 5 days: Rifampin 300mg PO BID x7days.
- Larkin S, Orthopedics 2008;31:37
Infection Risk Factors / Prevention
- Diabetes Mellitis: risk of infection increases with increasing glucose levels. Strict perioperative glucose control should maintain levels 200mg/dl. (Golden SH, Diabetes Care 1999;22:1408).
- Urinary tract infection: Chronic uncorrectable UTI should be managed with antibiotic suppression, and is relative contra-indication to elective surgery.
- Chronic renal failure: Patients on dialysis should recieve hemodialysis the day before elective surgery. Prior renal transplant patients are not at as high a risk of infection as dialysis patients.
- Rheumatoid Disease: RA medications such as penicillamine, indomethacin, cyclosporine, choroquine and prednisolone have been shown to increase the risk of surgical site infection.
- Immunocompromise:
- Smoking: Cessation of smoking during the peri-operative period decreases the risk of surgical site infection. (Craig S, Plas Reconstr Surg 1985;75:842).
- Medical Problems (HTN, CAD, COPD, etc)
- Blood Transfusion: In patients undergoing hip replacement or spine surgery, the postoperative infection rate with allogeneic blood transfusion appears to be 7- to 10-fold higher than with autologous blood or no transfusion. (Blumberg N, Semin Hematol 1997;34:34). The need for allogeneic transfusions should be reduced by proper pre-operative planning.
- Hypothermia
- Obesity
- Malnutrition: Can be assessed by serum protein and albumin levels. Pre=operative nutritional supplementation has been shown to decrease infections rates (Synderman CH, Laryngoscope 1999;109:915).
Intraoperative Infection Factors
- Pre-operative antibiotics should be given within 30 minutes before surgery. (Classen DC, N Engl J Med 1992;326:337).
- Hair removal should be performed with electric clippers immediately before surgery.
- Risk of infection increases as the number of people in the OR increases. (Pryor F, AORN J 1998;68:649).
- Laminar air flow and keeping the doors closed during surgery reduces risks of infection. (Ritter MA, CORR 1999;369:103).
- The length of surgery correlates with the infection rate.
Infected IM nail
- treatment generally requires exchange nailing with reaming of canal and 6wks IV antibiotics
- Healed fx with infected IM nail=mail removal, reaming, antibiotic nail placement. Use high dose antibiotic cement; 3.6g tobramycin and 10g vancomycin per 40g of bone cement. (Penner MJ, J Arthroplasty 1996;11:939). fill large chest tube with antibiotic cement, place guide wire in center of cement. Remove chest tube once cement hardens, then place nail.
Coagulase postive staph = Staph aureus
Coagulase negative staph = staph epidermidis
Septic Arthrits (Adult)
Prophylaxis Recommendations
- Cefazolin dosing is 2 g for adult patients or 3 g when the weight is greater than 120 kg every 4 hours. Pediatric dosing is 30 mg/kg. May Consider Cefuroxime 1.5g IVPB.
-
Clindamycin dosing is 900 mg in adult patients every 6 hours. Pediatric dosing is 10 mg/kg.
-
Vancomycin dosing is 15 mg/kg and needs to be administered 60 to 120 min before incision to achieve minimum inhibitory concentration.
- For MRSA colinization / high MRSA rate institutions or PCN allergic patients: Vancomycin 1g IVPB. Consider intranasal mupirocin ointment.
- IV antibiotics started withing 1 hour of surgical incision and completed before tourniquet is inflated.
- For obese patients antibiotic dose should be increased appropriately (Ancef 2g IVPN OCTOR). (Forse A, Surgery 1989;106:750).
- Prophylactic antibiotics shouldbe discontinued within 24 hours of the end of surgery.
- AAOS Post Arthroplasty Antibiotic Prophylaxis recommendations for elective procedures.
Penicillin Allergy
- Penicillin allergies are reported by up to 15% of the US population. 95% of these allergies do not correspond to a true allergy when tested
- Low Risk Penicillin Allergy: Side effects/intolerances (GI symptoms, headache, muscle aches, or psychiatric disturbances) Limited hypersensitivity reactions (self-limited cutaneous rash, urticaria .5 yr ago, or itching) Nonspecific (unknown reaction, or remote childhood reaction). Recommend give cefazolin
- Moderate Risk Penicillin Allergy: Disseminated hypersensitivity or anaphylaxis (swelling of the face or throat, angioedema, difficulty breathing, or urticaria ,5 yr ago): Recommend allergy skin testing or give Vancomycin or clindamycin.
- High Risk Penicillin Allergy: Stevens–Johnson syndrome or toxic epidermal necrolysis (diffuse ulceration, blistering, or pustulosis). Multiorgan hypersensitivity response (history of kidney or liver injury). Recommend give Vancomycin of clindamycin.
- Sarfani S, J Am Acad Orthop Surg 2022;30:e1-e5
Infection Work-up
- CBC with differential, ESR (rises within 2 days, continues to rise for 3-5 days even with treatment), CRP (rises witin 6 hours, peaks at 48 hrs, normal witin 1 week), blood cultures, gram stain, CXR. Consider Acid-fast staining, fungal cultures, prolonged incubation times (especially fro infections after arthroscopic surgery).
- Serum IL-6 is indicative of early periprosthetic infection (DiCesare PE, JBJS 2005;87A:1921).
- Xray: demonstrate soft-tissue swelling / loss of tissue planes early. Bone abnormalities require 30-40% bone losss.
- MRI: highest sensitivity and specificity for infection / osteomyelitis. low signal intensity in bone marrow on T1 images may indicated osteomyelits (bone marrow normally has high-signal intensity on T1 images).
- Bone scan: technetium 99m; gallium citrate Ga 67; indium-111 leukocyte-labeled etc.
Lyme Disease
- Most common vector-borne infection in the US.
- Etiology: spirochete Borrelia burgdorferi; transmitted by infected ticks.
- Common locations: Northeast, Northwest, Midwest rural wooded areas.
- Stage 1 (localized infection): skin lesion with expanding erythema migrans. RX= Doxycycline 100mg PO BID times 20 days.
- Stage 2 (disseminated infection): hematogenous spread (meningitis, neuritis, carditis, AV node block, musculoskeletal pain. RX= Doxycycline 100mg PO BID times 30 days.
- Stage 3 (persistent infection): intermittent/chronic arthritis, encephalopathy, acrodermatitis.
- Diagnosis: enzyme-linked immuosorgent assay and Western blot testing. May be negative in first several weeks of disease. Consider spirochete culture from synovial fluid or skin lesion. RX= Doxycycline 100mg PO BID times 60 days.
- Alternative antiobiotics: Amoxicillin 500mg PO QID, Cetriazone 2g IVPB daily for 14-28 days or Penicillin G 24million units daily or 14-28 days.
- Vaccination is available for patients in high risk areas.
Infection s/p ORIF
- Perioperative period: I&D with antibiotic treatment. May consider conversion to external fixation.
- Prior to fracture healing: if implants are stable generally treat with supressive antibiotics, wound coverage and implant removal after bone healing.
- After fracture union: implant removal, antibiotics.
|

