|
|
synonyms: HTO, high tibial ostetomy
HTO CPT
HTO Anatomy
- the peroneal nerve is closely adherent to the periosteum of the fibula, particularly at the most proximal few millimeters of the fibula and at points located in the segment of bone between 70 and 153 mm from the fibular head. Therefore, a fibular osteotomy should be performed at least 160mm distal to the proximal tip of the fibular head to avoid damage to the peroneal nerve. (Mont, MA, JBJS 1996;78A:863)
HTO Indications
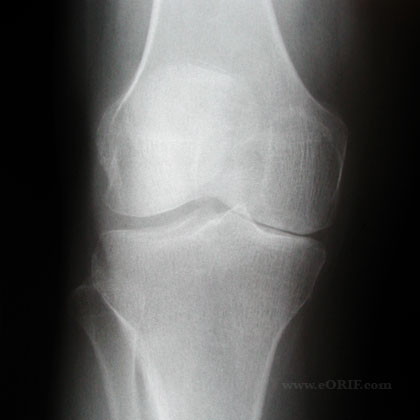
- Isolated medial compartment DJD with varus deformity <17.5degrees, without joint subluxation (joint subluxation indicates collateral ligament instability (high adductor moment) and is associated with poor HTO outcomes.)
- Ideal patient is physiologically, young and active, <50y/o.
- OCD of the medial femoral condyle in an adult (Slawski DP, Clin Orthop 1997;341:155)
- Osteonecrosis of the medial femoral condyle in a young active patient. (Koshino T, JBJS 1982;64A:47)
- Posterolateral Instablility
- Chondral Injury
- Patient undergoing ACL reconstruction with a varus knee.
HTO Contraindications
- Flexion contracture >15 degrees, ROM less than 90 degrees.
- Lateral compartment DJD
- Loss of the majority of the lateral meniscus
- Severe bone loss (<3mm)
- Patellar Baja
- Symptomatic Patellofemoral Arthritis
- Inflammatory Arthritis (rheumatoid)
HTO Alternatives
- Arthroscopic debridement-indicated for pt with ,1yr symptoms, nl alignment, mechanical symptoms.
- Unicompartmental knee- indications flexion cont <15, ROM >90, age >60, sedentary: rehab easier, costs less, quicker ROM, preserves ligamants/proprioception, 92% last 10yr, 15yrs = 60% working. Creates bone defect which often must be filed with allograft
- Total Knee Arthroplasty
- Distal Femoral Osteotomy-for valgus deformity <15, indications as above
- Knee Arthrodesis-indicated for infection, failed TKA, young active patients, soft tissue defects, absent extensor mechanism, neuropathic joint disease. fusion in 10-15 flexion and 0-7 valgus. complications=infection, non/malunion, pain.successful in 80-90% of failed condylar components, 55% of failed hinged prosthesis.
HTO Pre-op Planning / Considerations
- Generally considered a staging procedure for TKA. Indicated to delay TKA for 7-10 years and allow an active lifestyle during this time.
- draw line from center of femoral head to center of talus. This demonstrates the patients mechanical axis.
- 62.5% the width of the tibial plateau
- approximatley 1 degree of correction corresponds to 1mm of opening
- Evaluate lateral xray for patella baja which is a contraindication to opening wedge HTO.
- Ensure appropriate instrumentation is available including large staples if opposing cortex is inadvertently violated.
- Ensure patients symptoms are consistant with diagnosis. Patellofemoral pain in a varus knee will not be improved by an HTO.
- Technique options = medial opening-wedge or a lateral closing-wedge osteotomy. Medial opening-wedge osteotomy is contraindicated in smokers because of concern for nonunion.
- When performing concomittant HTO/ACL reconstruction the proximal screws must be placed so that the anterior screw diverges anteriorly and the posterior screw diverges posteriorly so that the screws will not interfear with the tibial tunnel for the ACL. Locking HTO plates can not be used as they do not allow screws to be placed divergently.
HTO Surgical Techniques
- Lateral Closing Wedge Osteotomy: Provides bone on bone contact with improved healing potential. (Billings A, JBJS 2000;82A:70)Increased risk of peroneal nerve injury.
- Medial Opening Wedge Osteotomy: Smaller incision, intra-operative adjustment more easily performed. Increased risk of nonunion/hardware failure.
- Dome Osteotomy: rarely used. (Korn MW, Am J Knee Surg 1996;9:12)
Opening Wedge Technique
- Pre-op antibiotics, supine, have c-arm ready
- EUA of knee
- Place well padded tourniquet high on the thigh
- Prep and drape R/L lower extremity in standard sterile fashion
- Perform standard knee arthroscopy
- Leg exsanginated with Eschmar bandage and tourniquet inflated
- 7 mm vertical incision over pes anserine insertion
- Sartorious fascia identified and insized longitudinally exposing the semitendinosis and gracillis
- Semitendinosis and gracillis retracted inferiorly
- Sufericial MCL is subperiosteally elevated from anterior to inferior keeping distal portion intact
- Blunt Homan retractors placed anteriorly and posteriorly, protecting surrounding structures. Ensure retractors are placed directly on bone.
- Osteotomy guide pins are placed under flouroscopic guidance. Pins should pass just proximal to tibial tubercle and stop just medial to lateral cortex. Ensure proximal fragment is at least 15mm thick to avoid intra-articular fracture.
- Cutting guide is placed and osteotomy is performed under fluoroscopic guideance. Stop 1cm medial to the lateral cortex to ensure lateral cortex is not bridged.
- Osteotomy site is opened to pre-determined level with wedge or osteotomy hinge. Appropriate opening is verified fluoroscopically with long alignment rod, or electro-cautery cord placed from hip to ankle.
- If at any time the lateral cortex is bridged the osteotomy should be closed and the lateral cortex stapled through a minimal lateral incision.
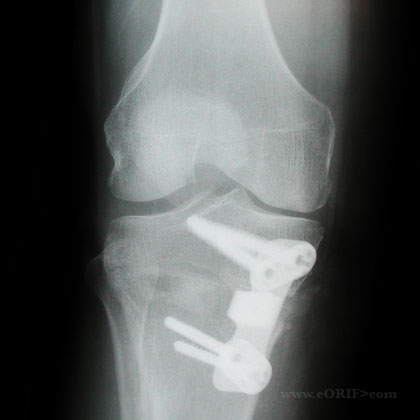
- Osteotomy plate is place and screwed in place using standard AO techniques
- Interveing space is filled with bone graft. Cortical bone graft should be used for any defect >7.5mm.
- Irrigate.
- Incision closed in layers
- Post-operatively patient is placed in hinged knee brace, NWB for 4-6 weeks.
HTO Complications
- Cosmesis: A varus knee will be converted to a valgus knee during a HTO and may be consider a cosmetic deformity by some patients. This should be discussed with all patients pre-operatively as part of the informed consent.
- Infection
- Patella Baja: associated with anterior knee pain and technically difficult TKA conversions. (Scuder GR, JBJS 1989;71:245). The incidence can be decreased by avoiding post-operative immobilization. (Westrich GH, CORR 1998;354:169)
- DVT/PE
- Delayed Union
- Nonunion: less common after lateral closing wedge than medial opening wedge. Avoid medial opening wedge osteotomy if large correction is needed, or if patient is a smoker or diabetic.
- Fracture (tibial plateau)
- Peroneal nerve palsy(more common after lateral closing wedge osteotomy.
- Compartment Syndrome
- Under / Over correction
- Arterial Injury
- Arthrofibrosis
- Loss of correction / fixation
- Painful hardware
HTO Follow-up care
- Post-op:
- 7-10 Days:
- 6 Weeks:
- 3 Months:
- 6 Months:
- 1Yr:
HTO Outcomes
- 85% survivorship at five years, 53% at ten years with conversion to TKA as endpoint. (Billings A, JBJS 2000;82A:70).
HTO Review References
- Wright JM, JAAOS 2005;13:279
- Rossi R, Bonasia DE, Amendola A. The role of high tibial osteotomy in the varus knee. JAAOS. 2011 Oct;19(10):590-9.
- Sprenger TR, Doerzbacher JF. Tibial osteotomy for the treatment of varus gonarthrosis. Survival and failure analysis to twenty-two years. J Bone Joint Surg Am. 2003 Mar;85-A(3):469-74. Erratum in: J Bone Joint Surg Am. 2003 May 85-A(5):912.
- Amendola A. Knee osteotomy and meniscal transplantation: indications, technical considerations, and results. Sports Med Arthrosc. 2007 Mar;15(1):32-8.
- Noyes FR, Barber-Westin SD, Hewett TE. High tibial osteotomy and ligament reconstruction for varus angulated anterior cruciate ligament-deficient knees. Am J Sports Med. 2000 May-Jun;28(3):282-96.
- Rossi R, Bonasia DE, Amendola A. The role of high tibial osteotomy in the varus knee. J Am Acad Orthop Surg. 2011 Oct;19(10):590-9.
- °
|