|
|
synonyms: calcium pyrophosphate deposition disease, CPPD, pseudogout, podagra, crystaline deposition disease
Pseudogout ICD-10
- M11.20 Other chondrocalcinosis, unspecified site
- M11.211 Other chondrocalcinosis, right shoulder
- M11.212 Other chondrocalcinosis, left shoulder
- M11.221 Other chondrocalcinosis, right elbow
- M11.222 Other chondrocalcinosis, left elbow
- M11.231 Other chondrocalcinosis, right wrist
- M11.232 Other chondrocalcinosis, left wrist
- M11.241 Other chondrocalcinosis, right hand
- M11.242 Other chondrocalcinosis, left hand
- M11.251 Other chondrocalcinosis, right hip
- M11.252 Other chondrocalcinosis, left hip
- M11.261 Other chondrocalcinosis, right knee
- M11.262 Other chondrocalcinosis, left knee
- M11.271 Other chondrocalcinosis, right ankle and foot
- M11.272 Other chondrocalcinosis, left ankle and foot
- M11.28 Other chondrocalcinosis, vertebrae
- M11.29 Other chondrocalcinosis, multiple sites
- See all chondrocalcinosis ICD-10 codes
Pseudogout ICD-9
- 712.2(chondrocalcinosis due to pyrophosphate crystals, site unspecified)
- 712.21 (shoulder region)
- 712.22 (upper arm)
- 712.23 (forearm)
- 712.24 (hand)
- 712.25 (pelvic region and thigh)
- 712.26 (leg)
- 712.27 (ankle and foot)
- 712.28 (other specified site)
- 727.82 (calcium deposites in tendon and bursa)
- 712.3 Chondrocalcinosis, unspecified
- 275.4 Disorders fo calcium metabolism
Pseudogout Etiology / Epidemiology / Natural History
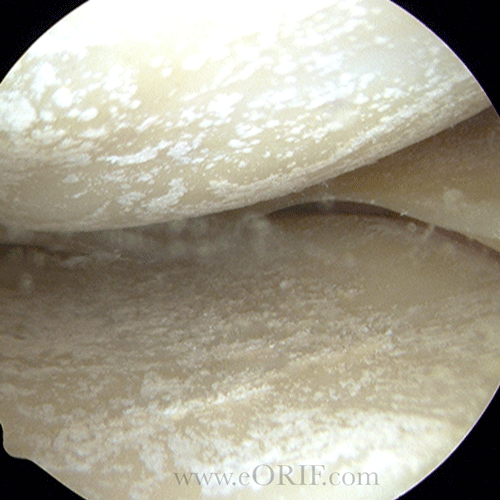
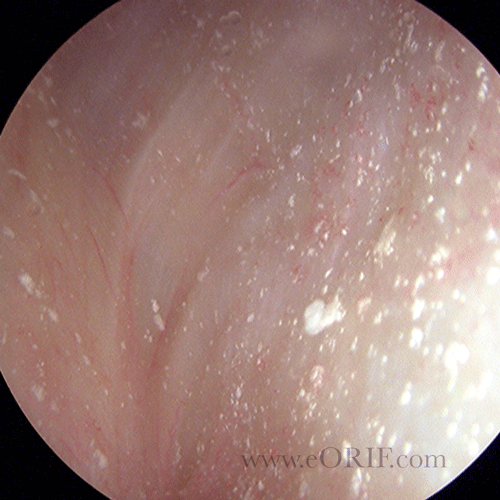
- Caused by calcium pyrophosphate deposition in joints.
- May lead to scapholunate advanced collapse in the wrist.
- Chondrocalcinosis = calcification of the articular cartilage or meniscus. Usually occurs in the periphery. More common in women. Incidence increases with age.
Pseudogout Anatomy
- May affect any joint: 50% occurs in the knees. Generally occurs in larger joints. sternoclavicular joints etc.
Pseudogout Clinical Evaluation
- Acute severe pain in a single joint without antecedent trauma.
- Pain, warmth, tenderness, erythema of affected joint.
Pseudogout Xray / Diagnositc Tests
- Xrays: demonstrate chondrocalcinosis of the menisci or articular cartilage.
- Joint aspiration: Fluid sent for cell count, gram stain and cultures. Calcium pyrophosphate crystals are weakly positive birefringent rhomboid-shaped crystals.
Pseudogout Classification / Treatment
- Consider NSAIDs and corticosteroid injections.
- Exercise, weight loss and canes may be beneficial
Pseudogout Associated Injuries / Differential Diagnosis
- Associated with: hyperparathyroidism, hemochromatosis, hypophosphatasia and hypothyroidism
- Gout
- Osteoarthritis
- Rheumatoid arthritis
- Charcot arthropathy
- Cellutis
- Septic Joint
- Lyme disease
Pseudogout Complications
Follow-up Care
- Generally managed by PCP/rheumatologist long-term.
Pseudogout Review References
- Fisseler-Eckhoff, Arthoscopy 1992;8:98.
- °
|


