 |
synonyms: ulnocarpal abutment, ulnolunate abutment, ulnotriquetral abutment, ulncarpal impingement
Ulnocarpal Impaction Syndrome ICD-10
- M24.831 - Other specific joint derangements of right wrist, not elsewhere classified
- M24.832 - Other specific joint derangements of left wrist, not elsewhere classified
- M24.839 - Other specific joint derangements of unspecified wrist, not elsewhere classified
Ulnocarpal Impaction Syndrome ICD-9
- 715.13 (Osteoarthritis localized, primary, forearm)
- 718.83(other derangement of joint, not elsewhere classified, forearm.
Ulnocarpal Impaction Syndrome Etiology / Epidemiology / Natural History
- Ulnolunate abutment is between the ulnar articular seat and the lunte.
- Ulnotriquetral abutment is between the ulnar styloid and the triquetrum.
Ulnocarpal Impaction Syndrome Anatomy
- Load bearing across the wrist: 82% radius, 18% ulna in neutral postion. Ulnar shortening to 2.5mm ulnar minus reduces ulnocarpal forces to 4%. (Palmer AK, CORR 1984;187:26)
Ulnocarpal Impaction Syndrome Clinical Evaluation
- Insidious or abrupt ulnar sided wrist pain
- Pain exacerbated by activities especially repetitive forearm rotation and gripping
- TFCC tenderness, pro/sup with clenched fist and ulnar deviation exacerbates symptoms, pain with compressing radioulnar joint during sup/pro=DRUJ arthritis
Ulnocarpal Impaction Syndrome Diagnositc Tests
- P/A and lateral wrist xrays
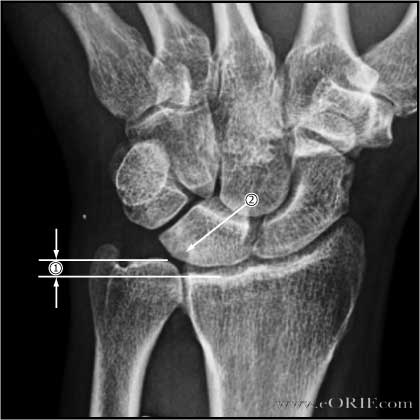
- Ulnar variance: determined on neutral rotation P/A view. Measured by drawing a transverse line at the level of the lunate fossa and a second transverse line at the level of the ulnar head, and determining the distance between the two lines. Positive ulnar variance increases with power grip and pronation. Consider pronated grip view. (Tomaino MM, J Hand Surg 2000;25Am:352). Normal = neutral (articular surface of distal ulna and radius equal). Postive (ulna longer) associated with ulnocarpal impaction, lunotriquetral ligament injurie and TFCC tears. Negative (ulna shorter) associated with carpal instability, Keinbock's disease.
- Ulnocarpal impaction is indicated by cystic / sclerotic lesions in the lunate and proximal medial ulna best seen on the P/A view.
Ulnocarpal Impaction Syndrome Classification / Treatment
- Activity modification, NSAIDS, splints
- If non-operative treatment fails, consider corrective radial osteotomy for distal radial malunion: ulnar shortening osteotomy (Milch H JBJS 23A:311;1941), wafer procedure for positive unlar variance <4mm(Feldon P, J Hand Surg 17A:731;1992)
Ulnocarpal Impaction Syndrome Associated Injuries
- Lunotriquetral ligmanet tear
- TFCC
- Distal radius malunion
- Radial head resection
- Premature distal radial physeal closure
Ulnocarpal Impaction Syndrome Complications
- Nonunion (@5%)
- Pain
- Stiffness
- Painful hardware
- DRUJ incongruity / arthritis
- Dorsal sensory branch of ulnar nerve injury.
Ulnar Shortening Osteotomy Follow-up care
- 7-10 follow-up:
- 6 week follow-up:
- 12 week follow-up: check xrays
- Post-op: volar splint, sling, NWB, elevation, digital ROM exercises
- 7-10 Days: dressing changed, removable volar splint placed. Start OT for ROM.
- 6 Weeks: check xrays. Advance therapy. Discontinue removable splint and advance to strengthening once bony union is evident.
- 3 Months: Advance strengthening, work on any ROM deficits. Consider bone stimulatorif union is not evident.
- 6 Months: follow-up xrays. Return to unrestricted activity.
- 1Yr: follow-up xrays, assess outcomes.
- Wrist outcomes.
Ulnocarpal Impaction Syndrome References
Green's Operative Hand Surgery: 2-Volume Set , 6e, 2010 |

