|





|
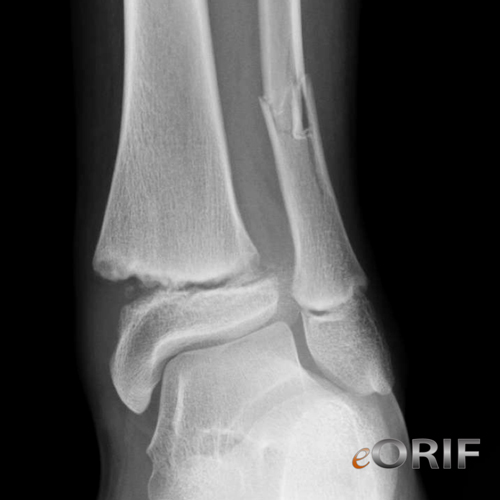
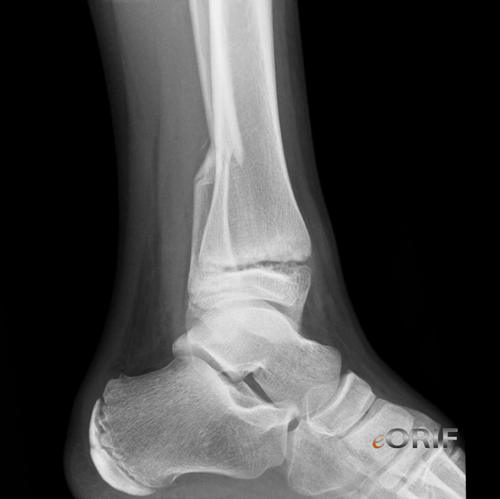
synonyms:pediatric distal tibia fracture, pediatric ankle fracture, pediatric medial malleolus fracture
Pediatric Distal Tibial Physeal Fracture ICD-10
A- initial encounter for closed fracture
B- initial encounter for open fracture type I or II
C- initial encounter for open fracture type IIIA, IIIB, or IIIC
D- subsequent encounter for closed fracture with routine healing
E- subsequent encounter for open fracture type I or II with routine healing
F- subsequent encounter for open fracture type IIIA, IIIB, or IIIC with routine healing
G- subsequent encounter for closed fracture with delayed healing
H- subsequent encounter for open fracture type I or II with delayed healing
J- subsequent encounter for open fracture type IIIA, IIIB, or IIIC with delayed healing
K- subsequent encounter for closed fracture with nonunion
M- subsequent encounter for open fracture type I or II with nonunion
N- subsequent encounter for open fracture type IIIA, IIIB, or IIIC with nonunion
P- subsequent encounter for closed fracture with malunion
Q- subsequent encounter for open fracture type I or II with malunion
R- subsequent encounter for open fracture type IIIA, IIIB, or IIIC with malunion
S- sequela
Pediatric Distal Tibial Physeal Fracture ICD-9
- 823.80 (closed fracture of unspecified part of tibia)
- 823.81 (unspecified part, closed, fibula with tibia)
- 823.90 (open fracture of unspecified part ot tibia)
- 823.92 (open unspecified part, fibula with tibia)
Pediatric Distal Tibial Physeal Fracture Etiology / Epidemiology / Natural History
- twisting mechanism to the lower leg during sports or recreation.
- Ankle injuries are very common in children and adolescents and second only to wrist and hand injuries
Pediatric Distal Tibial Physeal Fracture Anatomy
- Distal tibial growth plate closure starts anteromedially, progresses posteriorly and laterally and finishes anterolaterally.
- Ankle ligaments (deltoid ligament, posterior talofibular ligament, calcaneofibular ligament, and anterior talofibular ligament; posterior tibiofibular ligament and anterior tibiofibular ligament) are generally stronger than the growing physis; thus, osseous injury is more common then ligamentous injury in children and adolescents.
- Distal tibial physis accounts for 45% of tibial growth.
- Distal tibial growth continues until age 14 years in girls and age 16 years in boys.
- Distal tibial physis closure starts centrally, followed by closure anteromedially and posteromedially and finishes laterally.
Pediatric Distal Tibial Physeal Fracture Clinical Evaluation
- Pain and deformity in the ankle, inability to bear weight, ankle swelling, ecchymosis, degree dependent on fracture severity.
- Evaluate skin integrity, swelling, and neurovascular status of the leg/foot.
Pediatric Distal Tibial Physeal Fracture Xray / Diagnositc Tests
- A/P, lateral and mortise views of the ankle.
- CT: consider for intra-articular fractures
- MRI generally not indicated although can provide information on ligamentous and physeal injury. (Lohman M, Skeletal Tadiol 2001;30:504).
Pediatric Distal Tibial Physeal Fracture Classification / Treatment
- Salter-Harris Type I: approximately 15% of distal tibial physeal fractures. Low incidence of physeal arrest. The physis is disrupted through the zone of hypertrophy. Nondisplaced (step-off of <2 mm): long leg NWB cast for 3 weeks followed by short leg cast, WBAT for 3-4 weeks. Displaced (step-off of >2 mm): Closed reduction under general anesthesia with muscle relaxation (decreased risk of iatrogenic physeal injury). Incomplete reduction suggests interposed peristeum which may lead to premature physeal closure required open reduction. (Barmada A, JPO 2003;23:733). Open reduction indicated if 2 attempts at closed reduction are unsuccessful. Internal fixation rarely needed. Residual physeal gap of ≥3 mm risks premature physeal closure.
- Salter-Harris Type II: approximately 40% of distal tibial fractures. Fracture through the zone of hypertrophy exiting through the metaphysis. Thurston-Holland fragment = triangular flake of metaphyseal bone carried with the epiphysis. Nondisplaced (step-off of <2 mm): long leg NWB cast for 3 weeks followed by short leg cast, WBAT for 3-4 weeks. Displaced (step-off of >2 mm): Closed reduction under general anesthesia with muscle relaxation (decreased risk of iatrogenic physeal injury). Incomplete reduction suggests interposed peristeum which may lead to premature physeal closure required open reduction. (Barmada A, JPO 2003;23:733). Open reduction indicated if 2 attempts at closed reduction are unsuccessful. Internal fixation rarely needed. Residual physeal gap of ≥3 mm risks premature physeal closure.
- Salter-Harris Type III Fracture: approximately 25% of distal tibial fractures. Fracture extends through the physis and exits through the epiphysis. Risk of joint incongruity and growth disturbance. Non-displaced (<2mm) = long leg non–weight-bearing cast for 4 weeks, followed by boot for 4 weeks. Displaced (>2mm) = ORIF. Medial approach medial malleolar fractures; anterolateral approach for Tillaux fractures. Avoid fixation across the physis or use smooth pins that cross the physis. Physeal pins removed as soon as fracture is stable
- Salter-Harris Type IV Fracture: appoximately 25% of distal tibial fractures. Fracture traverses the metaphysis, physis, and epiphysis. Triplane fractures and shearing injuries to the medial malleolus. Nondisplaced fractures= NWB long leg casts for 4 weeks, followed by NWB or SLC boot for 2 weeks. Displaced (>2 mm) = ORIF to minimize articular incongruity and physeal bar formation. Consider metaphyseal and epiphyseal screw. Associated fibular fractures typically are Salter-Harris type I/II injuries and are usually stable following reduction of the tibial fracture Consider ORIF of fibular fracture if unstable under fluoroscopy.
- Salter-Harris Type V Fracture: Uncommon. Compressive forces across the physis. Difficult to diagnose on initial radiographs. May develop growth arrest. Consider excision of the damaged portion of the physis and placement of fat graft. May development limb-length discrepancy or angular deformity.
- Salter-Harris Type VI Fracture: rare. Perichondrial ring injury; Non-displaced (<2 mm) = long leg non–weight-bearing cast for 4 weeks, followed by boot for 4 weeks. Displaced (>2mm) = ORIF or CRPP. High risk of physeal growth arrest.
Pediatric Distal Tibial Physeal Fracture Associated Injuries / Differential Diagnosis
- Triplane Ankle Fracture
- Juvenile Tillaux Ankle Fracture
- Adolescent Pilon Fracture
- Incisural Ankle Fracture
Pediatric Distal Tibial Physeal Fracture Complications
- Delayed union, nonunion
- Malunion
- Growth arrest
- Arthritis
- Osteonecrosis of the distal tibial epiphysis
- Compartment syndrome
Pediatric Distal Tibial Physeal Fracture Follow-up Care
- Follow-up xrays every 6 months for 2 years or until skeletal maturity to assess for physeal damage and deformity.
Pediatric Distal Tibial Physeal Fracture Review References
|







