|
synonyms: lateral malleolus fracture, ankle fracture Lateral Malleolus Fracture ICD-10
Lateral Malleolus Fracture ICD-9
Lateral Malleolus Fracture Etiology / Epidemiology / Natural History
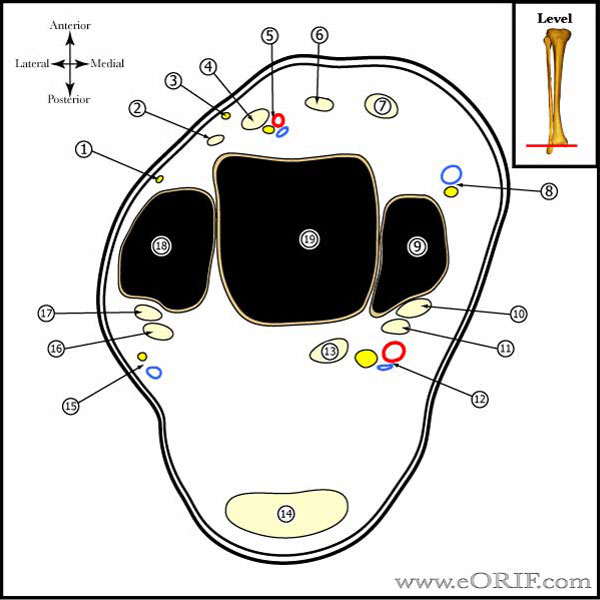
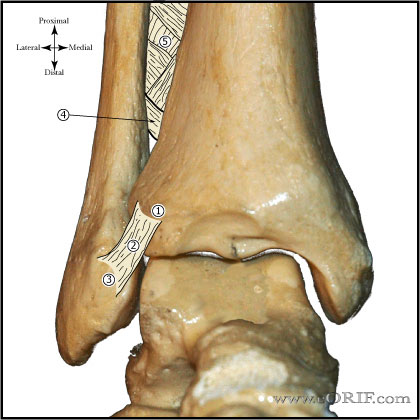
Lateral Malleolus Fracture Anatomy
Lateral Malleolus Fracture Clinical Evaluation
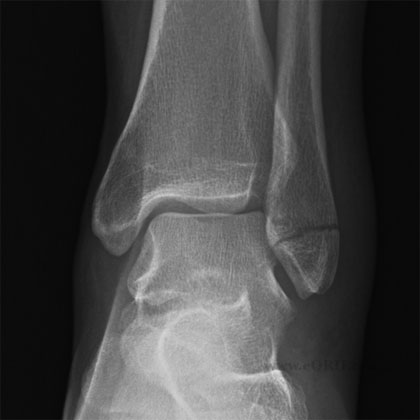
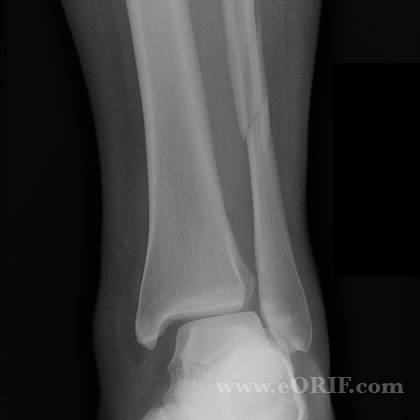
Lateral Malleolus Fracture Xray
Lateral Malleolus Fracture Classification/Treatment
Lateral Malleolus Fracture Associated Injuries
Lateral Malleolus Fracture Complications
Lateral Malleolus Fracture Follow up care
Lateral Malleolus Fracture References
|