|

|
synonyms: hip DJD, hip osteroarthritis
Hip Arthritis ICD-10
Hip Arthritis ICD-9
Hip Arthritis Etiology / Epidemiology / Natural History
Hip Arthritis Anatomy
Hip Arthritis Clinical Evaluation
- Groin pain exacerbated by hip internal rotation.
- Duchene sign = pt leans to the affected side while in stance phase of gait; indicates hip pathology.
- Loss of motion suggests intra/juxta-articular process
- Patrick's test: Groin pain with forcing hip into figure-of-4 postion, indicates hip pathology
- Stinchfield test: resisted straight leg raise causes groin pain, indicates hip pathology
- Labral pathology indicated by palpable click with moving from flexion/IR/adduction to extention/ER/abduction
- Snapping: Iliopsoas tendon snaps over iliopectineal eminence when flexed hip is extended with pt supine. Iliotibial band snaps over greater trochanter when standing pt rotates the adducted hip in stance phase.
Hip Arthritis Xray / Diagnositc Tests
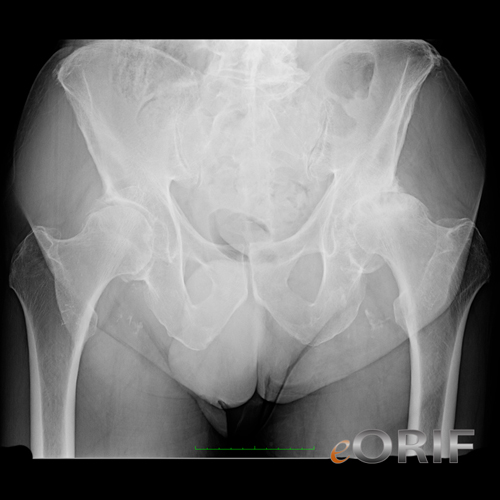
- AP pelvis, cross-table lateral hip, AP hip c leg internally rotated 15. Osteoarthritis demonstrates joint space narrowing, sclerosis, osteophytosis (classic triad). For other classic inflamatory arthitic findings see Xray Findings.
- Patients will likely have severe arthritis by age 65 if the Lateral Center-edge angle of Wibergis <16 degrees and the femoral head is uncovered >1/3.
- MRI: consider for patients with relatively normal xrays and potential Impingement Labral Tear, or osteonecrosis.
Hip Arthritis Non-operative Treatment
Hip Arthritis Operative Treatment
- Osteotomy: ideal candidate is >50y/o, normal weight, mechanical problem that can be corrected.
- Intertrochanteric osteotomy for femoral deformity (Perlau JBJS 1996;78A:1462)
- Periacetabular osteotomy for acetabular deformity
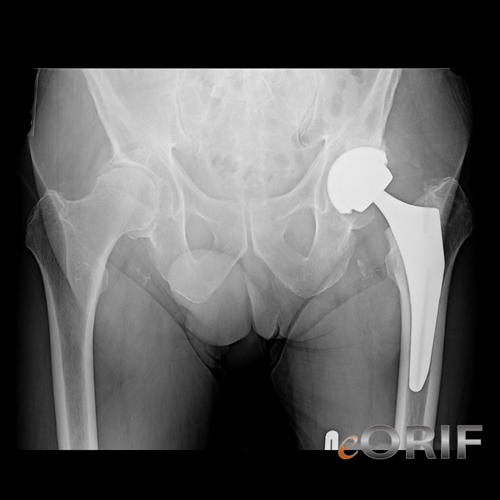
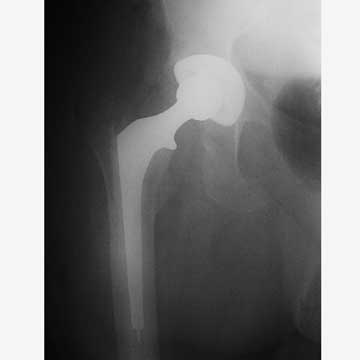
- Total Hip Arthroplasty
Hip Arthritis Associated Injuries / Differential Diagnosis
THA Complications
- THA Intra-op complications: fracture(Rx circlage wiring), neurovascular injury(common peroneal branch of sciatic= most common, results in foot drop)hypotension with cement insertion,
- main complications=death, dislocation, severe HO, infection, nerve palsy, leg length inequality.
- death In-hospital=0.1-0.8%, 30-day=0.15-1,42%, 90-day=0.2-0.74%: cause commonly cardiac or thrombeembolic
- Periprosthetic Infection: 0.2% (Mahomed NN, JBJS 2003;85A:27). Staph. aureus, streptoccocus, E. coli & Pseudomonas most common.
- osteolysis(polyethylene particles leading to an immune response(histiocytic) are classically implicated)
- loosening(indicated by symptoms, component migration/fracture, cement cracks, radiolucent zones circumferentially ), The acetabular cup is considered loose if there is >2mm radiolucency in all three zones(Fig. 4-3 Miller), progressive loosening in 1-2 zones, or change in position of the cup.
- Implant failure
- acetabular wear(rates less than 0.1mm/year expected, measured as in fig??)
- dislocation(1-4%of primary THA's, posterior more common) Risk factors=etoh, cerebral dysfunction
- nerve palsy=0.6-1.3% of primary THA, as many as 7.5% for revision. Sciatic most common (peroneal division) >femoral. Associated with women and limb lengthening >4cm(Lewallen, ICL JBJS 79A:1870,1997)
- Periprosthetic femur fx-Vancouver classification:type A=proximal to prosthesis: type B1=component solidly fixed, plating vs allograft strut; type B2=component loose, longer prosthesis; type B3=loose with poor bone, longer prosthesis+/-graft/cement; Type C=distal to prosthesis, treated independently
- Heterotopic bone formation(pt at risk=males c ankylosing spondylitis, DISH, posttraumatic arthtirits, past hx of heterotopic bone, occurs is 23% of pts with ankylosing spondylitis:indomethacin 75mg QD for 6wks vs single fraction dose about 700-800 rads given within 1-4 days postop had 2% incidence of H.O.(Lewallen DG: Heterotopic Ossification following total hip arthroplasty. Instr Course Lect 1995;44:287-292)
- DVT / PE
- Vascular injury-0.25%-external iliac artery and common femoral artery most common. (Lewallen, ICL JBJS 79A:1870,1997)
- Squeaking: metal on metal and ceramic THA's have been known to produce painless but audible squeaking with motion. Cause is unknown, but has not been reported to be associated with early failure or any specific problems.
Hip Arthritis Follow-up Care
Hip Arthritis Review References
|




