|
|
-
- Loss of stability / Graft failure: @10%
- Anterior knee pain / kneeling pain: 17.4%/100% BTB, 11.5% Hamstring
- Stiffness: 6.3%
- Painful hardware: 6.3%
- Infection: <2%
- Patellar fracture / patellar tendon rupture: <1% (BTB grafts)
- Arthritis: incidence after reconstruction is unkown
- Arthrofibrosis: rare
- Cyclops lesion: rare
- NVI (saphenous neuralgia): rare
- Complex Regional Pain Syndrome: rare
- Hemarthrosis
- Loss of stability / Graft failure, Anterior knee pain / kneeling pain, Stiffness, Painful hardware, Infection, Patellar fracture / patellar tendon rupture, Arthritis, Arthrofibrosis, Cyclops lesion, NVI (saphenous neuralgia), Complex Regional Pain Syndrome, Hemarthrosis
ACL Complications Review References
- CFreedman, KB, Complications of Anterior Cruciate Ligament Surgery, AAOS Mongraph Series 2005
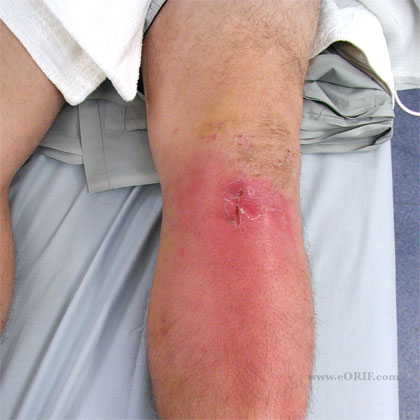
ACL Infection
- synonyms:
- ICD-9 =
- Incidence is <2%. 0.8% in a systematic review (Spindler KP, AJSM 2004;32:1986)
- Risk Factors: diabetes, prior surgery on affected knee, concomitant procedures. Diabetics have 18.8-times higher odds of postoperative infection after ACL reconstruction. (Brophy RH, JBJS 2015:97;450-4)
- Preventative measures: preoperative antibiotics, short surgery times.
- Offending organism is typically Staph aureus or Staph epidermidis.
- Contaminated cannulated instrumentation and graft tables have been implicated as causes of infection. Generally related to Coag Negative Staph. (Viola R, Arthroscopy 2000;16:), (Schollin-Borg M, Arthroscopy 2003;19:).
ACL Infection Clincal Evaluation
- Septic arthritis presents with: pain, temperature >100 F (38 C), effusion, warmth, painful limited ROM.
- ACL infection more commonly presents with reduced ROM noted in physical therapy, mildly increasing pain. Generally occurs in first 3 weeks post-operatively, but can occur at any time.
ACL Infection Work-up
- Immediate joint aspiration sent for anaerobic and aerobic cultures, gram-stain, cell count. WBC count is generally >50,000 with >90% polys
- ESR, CRP and WBC count with differential should be order. ESR and CRP are typically elevated for the first week after uncomplicated surgery.
ACL Infection Treatment
- Generaly presents with increaseing pain, erythema, poor motion within 2 weeks of surgery. Work-up = joint aspiration with Gram stain, cell count and differential, aerobic and anaerobic cultures; CBC, CRP, ESR.
- Common organisms: most common pathogen is coagulase-negative staph (Staphylococcus epidermidis), followed by Staph. aureus.
- Surgical Irrigation and debridement. All associated surgical wounds should be opened, irrigated and debrided. Partial or total synovectomy is indicated. The need for graft removal is controversial.
- Consider graft retention if infection was treated acutely, joint appeared benign and the graft was viable and stable. Successful treatment with graft retention has been reported. (Schollin-Borg M, Arthroscopy 2003;19:941). If possible any associated hardware should be exchanged or temporarily removed and sterilized.
- The graft and all hardware should be removed if diagnosis was delayed, or infection responds poorly to initial trial of graft retention.
- Empiric antibiotics are started after intra-operative cultures are taken. Final antibiotic treatment is determined based on sensitivities.
- Infections Disease consult recommended.
- Need for repeat I&D is controversial. Consider repeating arthroscopic I&D every 48 hours until cultures are negative.
ACL Infection Follow-up
- Post-operative rehabilition should focus on ROM. An arthrofibrotic reaction is not uncommon.
- Graft reimplantation can be done as early as 6 weeks after eradication of the infection. (Burks RT, AJSM 2003;31:414).
ACL Infection Review References
- Kovacic JJ in Complications of Anterior Cruciate Ligament Surgery, AAOS Mongraph Series 2005
ACL Stiffness
- Stiffness requiring manipulation under anesthesia or lysis of adhesions occurs in 6.3% of patellar tendon reconstructions and 3.3% of hamstring reconstructions. (Freedman KB, AJSM 2003;31:2)
- Stiffness which fails to resolve with aggressive PT by 2-3 months should be considered for arthroscopic lysis of adhsion, notchplasty, and/or manipulation
ACL Neurovascular Injury
- Infrapatellar branch of saphenous nerve (saphenous neuralgia): paresthesia in the anteromedial region of the lower leg and tenderness at the medial side of the knee without motor or reflex abnormalities. Can be confirmed by anesthetic blockade. Treatment = saphenous neurolysis. To minimize the risk of damage to the saphenous nerve during hamstring harvest, the knee should be flexed and the hip external rotated.(Bertram C, Arthroscopy 2000;16:763).
Cyclops Lesion
- Generaly presents approximately 4 months postoperatively with loss of extension associated with pain at terminal extension, crepitus, and grinding with attempted extension.
- Fibrous nodule occupying the intercondylar notch, presenting a mechanical block to full extension found at arthroscopy.
- Anterior placement of the graft, particularly on the tibia, results in injury to the graft and subsequent nodule formation.
- Treatment: arthroscopic removal of the nodule.
- Marzo JM Arthroscopy 1992;8:10-18
Loss of stability / Graft Failure
- KT-1000 >3mm or knee giving way occurs in approximately 10% of ACL reconstructions.
- Graft failure occurs in 1.9% of patellar tendon reconstructions and 4.9% of hamstring ACL reconstructions. (Freedman KB, AJSM 2003;31:2).
- More common in patients younger than 20 years old. (Webster KE, Feller JA, Leigh WB, Richmond AK. Younger patients are at increased risk for graft rupture and contralateral injury after anterior cruciate ligament reconstruction. Am J Sports Med. 2014 Mar;42(3):641-7.)
Arthritis
- ACL reconstruction decreases the risk of future meniscal tear and improves stability, but its effects on delaying or preventing arthritis are unknown.
Anterior knee pain, kneeling pain
- Anterior knee pain occurs in 17.4% of patellar tendon ACL reconstructions and 11.5% of hamstring ACL reconstructions. (Freedman KB, AJSM 2003;31:2)
- Non-operatively treated patients may have up 22% incidence of anterior knee pain. (Buss DD, AJSM 1995;23:160)
- Kneeling pain occurs in virtually 100% of bone-patellar tendon-bone autograft ACL reconstructions.
- May be related more to loss of motion and poor rehabilitation techniques than to graft choice. (Sachs RA, AJSM 1989;17:760).
ACL Painful Hardware
- The incidence of painful hardware significant enough for patients to undergo hardware removal is 5.5% for hamstring reconstructions and 3.1% for patellar tendon reconstructions. (Freedman KB, AJSM 2003;31:2)
- Typically results from tibial posts used for hamstring graft fixation.
- Treatment: hardware removal after the graft is fully incorporated, 8-12 months.
Patellar fracture / Patellar tendon rupture
- Generally related to overaggressive bone plug harvest during Bone-Patellar Tendon-Bone ACL reconstructions.
- Bone plugs should be 10mm wide, less then 7mm deep and removed without overzealous levering. Primary bone grafting, with canal reamings or from the proximal tibia, of the harvest site is indicated.
- Treatment: see Patellar fracture, Patellar tendon rupture.
ACL Arthrofibrosis
- Global arthrofibrosis is: loss of flexion and extension with fibrosis of the medial and lateral gutters and the suprapatellar pouch. (Dehaven KE, ICL 2003;52:369)
- Risk factors: poor preoperative ROM, graft malposition or overtensioning, inadequate notchplasty, associated meniscal repair, CRPS, infection, excessive post-operative immobilization.
- Increased incidence with reconstruction performed within 3 weeks of injury (Shelborne KD, AJSM 1996;24:857).
- Decreased incidence when preoperative extension is 10 degrees or better and initial post-operative bracing is in full extension, with motion starting with 24 hours. (Cosgarea AJ, AJSM 1995;23:87).
- Classification: Type 1 = < 10 degree extension loss and normal flexion; Type 2 = > 10 degree extension loss and normal flexion; Type 3 = > 10 degree extension loss and > 25 degree flexion loss with a tight patella; Type 4 > 10 degree extension loss, 30 degrees or more flexion loss, and patella infera with marked patellar tightness. (Shelborne KD, AJSM 1996;24:857).
- Treatment: Anterior scar resection down to the proximal tibia with medial and lateral capsular releases and knee manipulation; Notchplasty when necessary. Consider postoperative outpatient serial extension casting.
ACL Complications Review References
- Phelan DT, ICL 2006;55:465
|


